See all "Gut Yeast" Section Topics
Anal yeast infection can often be caused by yeast in the digestive system, or vagina, that has migrated to the anus. A classic symptom of an anal Candida infection, is intense itch in the perianal (in or around the anus) area. This itchiness can be exacerbated by the rubbing of underwear, pressure, and moisture in that area.
Secondly, intense burning of the anal region, can also result due to fungal invasion of that area. Also, sexual activity with a person with a penile yeast infection, or oral thrush, could lead to an anal yeast infection; if direct contact with an infected body part occurs. Consequently, if you do engage in anal sex, you should avoid doing this while yeast is present.
Although transmission of the yeast between sexual partners is unlikely, it can happen. So, to stop the cycle of repeated Candida infection, undergo a natural antifungal therapy and stop having anal sex until you recover.
One might wonder if homosexual males are more likely to develop an anal yeast infection; as frequent anal sex may aggravate the anus and allow for direct contact with a Candida infected penis. The answer is, according to a professional study we will discuss shortly, that sexually active homosexual males may have a very slight increase in anal Candidiasis occurrence; but, nothing too significant.
And, men who engage in anal intercourse, will likely will have a lower rate of balanitis (a yeast infection of the tip of the penis), while men who have vaginal intercourse, often have a more frequent occurrence of balanitis.
According to Karen Powell, in her article (published in Nursing and Residential Care [2012 14:12, 637-641]) on Candida infections in older adults, surface skin and mucous membrane problems due to these fungi, are very, very common. The types of common superficial yeast infections include: perianal dermatitis (irritation of the anus caused by something; in this case yeast), Candida balanitis, skin yeast infections, and intertrigo (an infection of skin folds).
So don’t feel like you are weird, or have an unusual problem—this type of thing happens to a lot of people.
Candida isn’t a bacteria; soap and water will not do much to dissuade this yeast’s development. And, over cleaning can worsen your anal irritation and pain. So, excessive cleaning isn’t going to do much; but, gently washing the anus after you pass a stool may help reduce itching. You will need to take out the Candida, and let the perianal area heal up, to get total relief.
It may sound unusual, but one medical text even reported that some people with severe anal itching commit suicide due to this problem. Natural medicine is very effective; and, you should be able to easily get rid of this problem using it!
A 1/2 Day & Yeast is Gone!
Linda Allen suffered from yeast infections for years. Through researching natural medicine & Candida, she found an efficacious solution!
Linda is one expert you want on your side! Let her show you how to get rid of a superficial yeast infection in just 12 hours; AND, keep it gone!
A 60-day, 100% money back guarantee is provided.
Visit Official Site!Candida and Anal Itching (Pruritus ani)
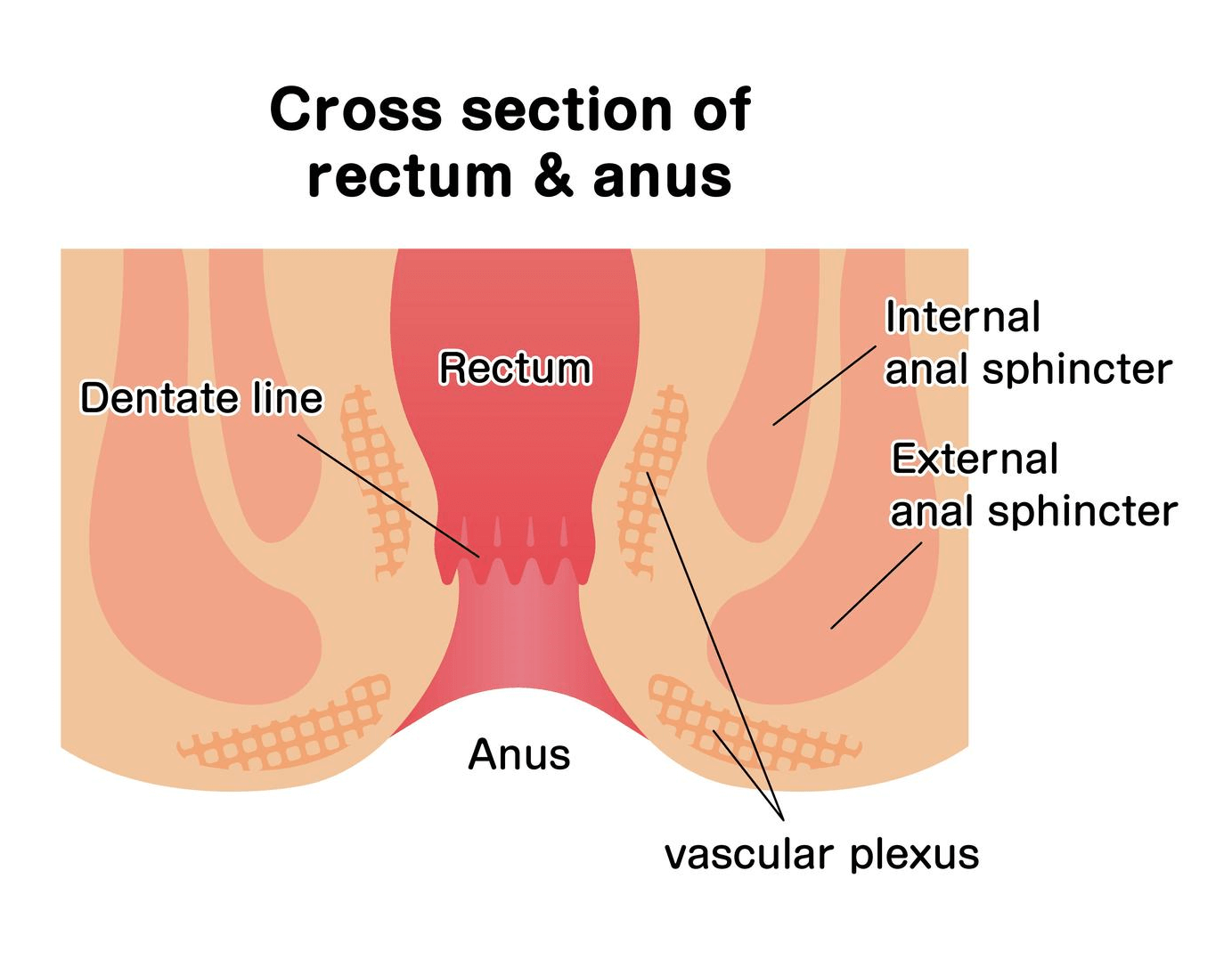
A relevant question to this topic, is: ”do males who engage in homosexual activity have a different rate of anal Candidiasis?” A study published in Genitourinary Medicine [73.5 (1997): 394-396] shows that the rate of anal Candidiasis is quite similar between heterosexual and homosexual men.
The study analyzed 223 heterosexual men and 193 homosexual men; each of these groups the men, had engaged in sexual activity within the last three months. 14% of heterosexual men and 18% of homosexual men had anal yeast infections. Of the varying types of yeast infections, there was a slightly elevated rate of various forms of Candidiasis among heterosexual men. The rate of penile Candida colonization was 16%. Of these 16% with male yeast infections, 27% of this fraction had balanitis, and 37% were symptomatic (meaning they had some noticeable problem due to the yeast).
Again, the researchers reported that those individuals who had anal intercourse had a lower occurrence rate of Candidal balanitis—as compared to the men who had vaginal intercourse (and, these practicing heterosexual men had a higher rate of Candidal balanitis). The most common symptoms, correlated with penile yeast infections, included burning and itching after sexual intercourse.
In vaginal yeast infections, itching around the vulva, and associated skin, is a common symptom. Candida can irritate the skin and cause itching where it occurs; and, if Candida is colonizing the anus, it can also cause anal itching. If you do scratch these itches, try and wash your hands immediately if they come into direct contact with the yeast. Although probably unlikely, you could spread the yeast to other areas of the body with your hands.
According to the authors of Improved Outcomes in Colon and Rectal Surgery, anal itching and irritation attacks men more than women; 4 men will get this condition for every 1 woman who does. Most people find that hot, humid weather makes this condition worse.
Exercise can also aggravate anal itching. Excessive scratching or cleaning of the anus can cause this condition to become even worse. Wearing close fitting clothing, or clothing made from fabrics that seal in air, also can cause this condition. However, if you notice white lesions or spots on the anus, these could be Candida lesions. Also, if you have a history of taking antibiotics, you are also going to be more likely to have anal itching caused by yeast.

A study, published in Wiener Klinische Wochenschrift [118.3-4 (2006): 90-94], found that Candidiasis was a prominent cause of anal itching and inflammation. The study was conducted over a 4 year time interval, and analyzed 126 individuals from both sexes. The individuals were aged from 7 to 82 years, and 57.1% of the patients in the study were males. All of those who participated in the study were presumed to have anal eczema. The patients had been experiencing anal irritation between 6 days and 120 months; over half had symptoms for at least 12 months.
A little under half (46%) of the patients, in the study, were presumed to have contact eczema. Note that in the study, the researchers made no distinction between intertrigo (inflammation of the skin folds by a pathogen) and specific Candidiasis. Some of the intertrigo was due to Candida, however. The study related that the most common type of anal infection is, in fact, a fungal infection. The study found the following disorders were responsible for the anal irritation and itching in the remaining half (54%) of patients:
- Intertrigo / Candidiasis (42.9%)
- Atopic Dermatitis (6.3%)
- Pruritus ani (5.6%)
- Psoriasis (3.2%)
- Skin Atrophy from Steroid Use (2.4%)
A study, published in the Annals of The Royal College of Surgeons of England [90.6 (2008): 457], cited research that indicated fungal infections were responsible for about 15% of all excessive anal itching. Consequently, yeast from the gut could be the cause of your anal itching; yet, chances are, most anal itching is not caused by Candida.
Even the study in Wiener Klinische Wochenschrift [118.3-4 (2006): 90-94] showed that Candida is not the cause for the majority of anal itching; as Candida likely, only accounted for a fraction of those who had intertrigo. However, if you’ve taken steroids, systemic antibiotics, or are diabetic; this would increase the probability of the cause being yeast.
Some of the symptoms of Candida causing anal infections and itching, taken from an article in Clinics in Colon and Rectal Surgery [17.4 (2004): 241], are given in the following quotation:
The yeast Candida albicans can cause both candidal intertrigo found between the gluteal folds and also a perianal dermatitis (anal inflammation and itching). These conditions can often be precipitated by use of oral antibiotic agents, steroid use, and pregnancy. Intertrigo (inflammation of the skin folds) develops in moist environments, causing pruritic, red patches with a fringe of “collarette” scale. There can also be associated small white pustules located near the patches, as well as “satellite” erythematous macules (red patches on smooth skin). Perianal candidiasis presents with pruritis ani and a more localized erythema (skin redness), around the anus.
Clinics in Colon and Rectal Surgery [17.4 (2004): 241]
Another study, published in the British Journal of Surgery [72.12 (1985): 967-969], demonstrates the prevalence of anal yeast infections. And, the study gives us an idea of how common Candida is as the cause for anal itching. Of the 174 proctological patients participating in this research who were experiencing anal itching, 21 of 77 were positive for Candida in their anus.
Of those patients who did not experience anal itching, 25 of 97 were positive for Candida. In total, about 26.4% of the proctological patients had an anal yeast infection. So, it is not absolute that anal itching always means Candida is the cause. It could be; however, there are other causes of anal itching that are beyond the scope of this article.
Anal Yeast Infection Symptoms & Causes

According to the book Andrews' Diseases of the Skin: Clinical Dermatology [Elsevier Health Sciences; 2015], anal yeast infections symptoms include: damaged skin, reddened skin, oozing of fluids, and these infections frequently causes anal itching (pruritus ani). In some cases, lesions around the primary infection (satellite lesions) can occur. In other instances, lesions do not appear. The authors also state that burning sensations and itching can become very severe.
Another book, Principles and Practice of Infectious Diseases [Elsevier Health Sciences; 2014], also discusses the symptoms and causes of anal yeast infections. According to the authors, the etiology of an itchy anus, can be any number of organisms; working alone or in congress. Yet, the book states that Candida is a very common cause of this condition. If not checked, the yeast can spread towards the scrotum or vulva. Symptoms of this problem include intense reddening of the skin and general damage to the skin.
The book, The ASCRS Textbook of Colon and Rectal Surgery [Springer Science & Business Media, 2011] also talks about anal yeast infections. According to the authors, this condition frequently causes bright red areas on the skin. Also, bumps with pus (more on yeast infection bumps) also form around the primary area of infection (known as satellite pustules).
The authors also state, that the causes of pruritus ani (anal itching) almost never happen just in the anal area alone; these causal diseases also regularly are harbored in other body locations. The book also cites a study that found that coffee consumption caused a reduction in anal resting pressure (the force the muscles use to contract while at rest) in about 73% of patients. A lowered anal resting pressure may lead to feces leakage; possibly one key cause of anal itching.
Another possible indicator of an anal Candida invasion, is the appearance of white patches or lesions on or around the anus. These lesions may bleed slightly when scraped away. The microscopic Candida fungi, that cause infections, are white in appearance. Thus, when a lot of yeast is colonizing an area, there can be white patches of yeast. This is a very powerful visual indicator, that you can look for at home, to help understand what is bothering your anal skin.
Eliminate Bacterial Vaginosis & Vaginal Odor
Jennifer O’Brien is one prominent expert on BV that knows how to get rid of vaginal odor. BV is a common infection that you don’t have to put up with.
Jennifer will show you how to naturally eliminate vaginal odor in just 3 days.
A 60-day, 100% money back guarantee is provided.
Visit Official Site!Naturally Cure Anal Yeast Infections

The solution to curing an anal yeast infection is quite similar to treating any type of external Candidiasis. A good natural solution to treating the anus is to mix various antifungal herbs and essential oils in honey and simply apply it to the anus. Keep in mind, that you should try and not add too much dry ingredients to the honey, as you want it to retain its viscosity.
Also, it would probably be best to apply the honey / herb mixture before you go to bed at night. That way, you can let the mixture stay in direct contact with the anus for a prolonged period of time. When you wake up in the morning, you can simply wash the honey / herb mixture off!
One thing to avoid at all costs when dealing with anal itching, is to try and not scratch too frequently or too vigorously. Excess, hard scratching of the anus, can only make the irritation worse; so, try and do less intense scratching! Also, excessive cleaning of the anus can further aggravate your itching.
Your problem is not a dirty anus, if it is Candida; and, excess washing only worsens this condition—no matter what the cause of it is. So, stop any extreme washing you may have been doing to resolve the itch—this is just making things worse.
You may want to try a strong concentration of tea tree oil mixed with a few drops of oregano oil and slightly diluted in some coconut oil. You can even also opt for aloe vera gel as a medium instead of coconut oil. Aloe vera is an adequate antifungal plant; so the gel alone will help to halt the spread of Candida. Aloe vera gel may be able to soothe the itch and any burning your are feeling in your anal region (more on aloe vera for Candida here).
Whatever medium you decide to go with, simply mix these oils up with the medium, and apply it to the anus. You should feel a soothing tingling sensation from the tea tree oil. And, the therapeutic effect of the essential oils and coconut oil will help to heal a wide array of pathogenic microorganisms that may be causing your itching—Candida included.
You might want to use an essential oil treatment a few times a day. This should help to consistently deliver antifungal phytochemicals to the Candida colonizing the anus. Of course, if you notice discomfort, reduce the frequency of application or stop altogether. By keeping up your chemical warfare in this manner, you should be able to expedite the healing of your anal skin.
Perhaps another critical therapy to undergo, especially if this isn’t your first anal yeast infection, is to eliminate Candida in the gut. Candida Hub’s gut yeast infection article describes how to naturally start cleansing the digestive system of Candida invaders. By restoring the dominance of probiotic bacteria in the gut, and eliminating excess yeast, you may eliminate the source of your recurrent anal Candida infections.
You can read more about gut yeast problems, and learn about a natural cleanse you can do to eliminate Candida in that area, to start restoring the health of your digestive system here: Gut Yeast Infections.
Essential Oils that Fight Candida & Itching
To target itching specifically, while you also combat Candida, you may want to choose essential oils that relieve itching and also possess antifungal ability. Fortunately, there are essential oils that perform both tasks; they may be ideal for you to use to clear up an anal yeast infection. These essential oils are chamomile and peppermint.
Lavender oil may also be a good choice for soothing itching due to its possible analgesic (pain relieving) action. Additionally, essential oils may be ideal to use for treating this condition as they may be rapidly absorbed through the skin (Koulivand, et. al; 2013).
Candida Hub has an entire article on essential oils that treat yeast infections and reduce the itch these infections cause. There you will find a recipe you can use as a template to make your own essential oil blend with a carrier substance. You can read this article here: Essential Oils for Yeast Infection Itch.
Clair Goodall: Author & Nature Lover
Clair Goodall is a bee-obsessed natural medicine convert from Minnesota. She is one expert you might want to know more about!
Clair will help you protect you and your family from toxic products and chemicals and help you discover solutions from nature.
Also, Clair’s book is backed by a 60-day, 100% money back guarantee
Visit Official Site!Literature on Anal Itching (Pruritus Ani)

Valerie Ann Worwood, in her book The Complete Book of Essential Oils and Aromatherapy, discusses pruritus ani (anal itching). Worwood states that this, of course, is a rather unglamorous problem with a varying etiology (cause). According to Worwood, anal itching can be caused by laxatives, antibiotics, the chemicals in toilet paper, clothing, and soap.
This book states that the anus can be an ideal environment for the proliferation of fungi and bacteria; due to the warmth and moisture content of the area. Also, hair in the anal area can pick up pathogens in the waste that exits the colon. Perspiration in this area can also lead to an itching anus.
Worwood suggests not using soap when washing the anus. Worwood also suggests using an essential oil bathing mixture to treat the area twice a day—preferably after passing stools. The following essential oil recipe is proposed by the book to treat anal itching:
- Geranium Oil — 5 Drops
- Lavender Oil — 4 Drops
- Bergamot Oil — 3 Drops
- Directions: Mix the essential oils together. Add two drops of the mixed essential oils to a bowl of water and wash the anus with it.
Anthony L. Komaroff and the Harvard Medical School, in their book The Harvard Medical School Family Health Guide, also discuss anal itching. According to the text, anal itching is an annoying and common health problem. They further state that anal itching is usually not a serious condition. Yet, anal itching can be something that a preexisting condition; such as allergies, psoriasis, anal fissures, or hemorrhoids; produce.
The book states that in most people, anal itching is a result of minor irritation; frequently caused by the use of scented soaps or toilet paper. The book suggests some home remedies to employ to relieve anal itching, some of them are the following:
- Wear loose cotton underwear for better air circulation
- Keep the anal area clean via washing with unscented soap and warm water. The area should then be dried gently; but get totally dry. This text suggests you can even use a blow dryer.
- Apply chilled witch hazel to the anal area.
- You can use an over-the-counter hydrocortisone cream (chamomile oil is a natural alternative to hydrocortisone).
- Try to limit how much you scratch; as scratching can cause further irritation to the area that may lead to more itching.
A Natural, 12 Hour Yeast Infection Cure

According to a research paper published in Clinical Microbiology Reviews [12.1 (1999): 80-96], Candida species are quite ubiquitous organisms. Candida are most frequently present in the mouth; and, live in 31% to 55% of healthy people. The species that causes approximately 70% to 80% of all Candida infections is C. albicans.
The Chinese Journal of Obstetrics and Gynecology [2011 Jul;46(7):496] reports there appears to be a correlation between intestinal Candida infections and vaginal yeast infections. And, this provides a clue, as to why yeast infections in general, can reoccur.
This study states, in 148 cases of vaginal candida infections, 33.1% of the women were infected in both the intestines and vaginal area. The recurrence rate of yeast infections, in women with simultaneous intestinal infection, was significantly higher than for women who did not have an intestinal infection. This study concluded that vaginal yeast infections are highly associated with simultaneous intestinal Candida infection.
As research appears to indicate, systemic Candida infections can and do happen. A more systemic Candida infection may primarily get a foothold in the intestines; and cause a wide array of problems. If your yeast infections keep happening, a systemic Candida problem may be why.
One woman who suffered from a systemic Candida infection, for about 12 years, was Linda Allen. The systemic Candida infection that attacked Linda caused a wide range of health problems in addition to yeast infections. Some of these problems, Linda describes in her own words in the following quote:
To be honest, it was hard to pinpoint exactly what was wrong: I wasn’t really sick, but I wasn’t really well either. I had listlessness, fatigue, brain fog, stomach ailments, unexplained rashes, skin infections, and so on. It seemed like every day brought a new challenge.
My energy was sapped and I felt exhausted, which affected my grades and put a big dent in my social life.
Linda Allen’s symptoms included an embarrassing vaginal discharge, severe itching, and burning sensations. Her infections were difficult to deal with, and Linda’s health problems cost her financially as well. Linda states these infections of Candida can become excruciating when they happen as frequently as a menstrual period.
Yet, Linda spent a great deal of time in research; and even questioned health professionals who were kind enough to share some time with her. Linda even tried an array of purported "cures." Although it took a while, eventually, Linda put together a natural treatment plan she hoped would solve her Candida situation.
After spending about a year refining her new approach, Linda tried her system on herself. It worked amazingly well. Linda even returned to a few medical doctors to get tested for the presence of infections. These tests revealed all indicators of infection had vanished! Linda was indeed well again, after such a long, difficult journey.
Linda has since published a book detailing how to copy her success. She also includes a 12 hour yeast infection cure that can get rid of a superficial (such as a genital yeast infection or oral thrush) yeast infection in about 12 hours.
Linda’s publisher protects those who get her book with a 60 day, 100% money back guarantee. Linda’s publisher, a subsidiary of the United States based firm Keynetics Incorporated, is a reputable digital retailer that has been around for a long time. They have great customer service, and make getting a full refund on Linda’s book quick and easy. If you’re not satisfied, you can quickly get all your money back.
If you would like to learn more about Linda’s journey to freedom from Candida, see reviews of others who tried her natural system, or find out more about her efficacious book; you can find more information at Linda Allen’s website.
Author: Mr. Nicholas Gross

Nick Gross is a natural medicine enthusiast who has been researching and writing about natural medicine since 2008. Nick is primarily a web developer but also researches and authors written and video content about natural health. Nick has a bachelor’s degree in Management Information Systems from the University of Northern Iowa.
Disclaimer
The information on this website is not a prescription for anyone. This information is for informational or educational purposes only, and is not a substitute for professional medical advice or consultations with healthcare professionals.
Affiliate Disclosure
Some of the links provided on this website are affiliate links. When a purchase is made through these links, Candida Hub earns money from commission. This helps to keep the website up and helpful to people for free. Thank you for any support!
Stay Up to Date
If you enjoyed this article, consider following / liking our Facebook page. This page is primarily utilized to alert followers of new articles that are put on Candida Hub. Candida related news is also discussed. While you are there, you can see what has been more recently added to Candida Hub.
SOURCES:
- http://dx.doi.org/10.12968/nrec.2012.14.12.637 — Karen Powell. “Candidiasis: fungal infections in older adults.” Nursing and Residential Care 2012 14:12, 637-641.
- http://dx.doi.org/10.1136/sti.73.5.394 — David, L. M., M. Walzman, and S. Rajamanoharan. "Genital colonisation and infection with candida in heterosexual and homosexual males." Genitourinary medicine 73.5 (1997): 394-396. PDF Available Here
- http://www.ncbi.nlm.nih.gov/pubmed/11360070 — Shihadeh, Awad S., and Ashraf N. Nawafleh. "The value of treating the male partner in vaginal candidiasis." Saudi medical journal 21.11 (2000): 1065-1067.
- Google Books — Whitlow, Charles B., et al., eds. Improved Outcomes in Colon and Rectal Surgery. Taylor & Francis, 2009. ISBN: 9781420071528
- http://dx.doi.org/10.1007%2Fs00508-006-0529-x — Kränke, Birger, et al. "Etiologic and causative factors in perianal dermatitis: results of a prospective study in 126 patients." Wiener Klinische Wochenschrift 118.3-4 (2006): 90-94.
- http://dx.doi.org/10.1308%2F003588408X317940 — Siddiqi, S., et al. "Pruritus ani." Annals of The Royal College of Surgeons of England 90.6 (2008): 457. Full Text Available Here
- http://dx.doi.org/10.1002/bjs.1800721210 — Dodi, G., et al. "The mycotic flora in proctological patients with and without pruritus ani." British journal of surgery 72.12 (1985): 967-969.
- http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2780053/ — McGirt, Laura Y., and Ciro R. Martins. "Dermatologic diagnoses in the perianal area." Clinics in colon and rectal surgery 17.4 (2004): 241.
- Google Books — William D. James, Timothy Berger, Dirk Elston. “Andrews' Diseases of the Skin: Clinical Dermatology.” Elsevier Health Sciences, 2015. ISBN: 0323319696.
- Google Books — John E. Bennett, Raphael Dolin, Martin J. Blaser. “Principles and Practice of Infectious Diseases.” Elsevier Health Sciences, 2014. ISBN: 9781455748013.
- Google Books — David E. Beck, et. al. “The ASCRS Textbook of Colon and Rectal Surgery: Second Edition.” Springer Science & Business Media, 2011. ISBN: 9781441915818.
- https://doi.org/10.1155/2013/681304 — Koulivand, Peir Hossein, Maryam Khaleghi Ghadiri, and Ali Gorji. "Lavender and the nervous system." Evidence-Based Complementary and Alternative Medicine [2013 (2013)].
- Google Books — Valerie Ann Worwood. “The Complete Book of Essential Oils and Aromatherapy.” New World Library, 1991. ISBN: 9780931432828
- Google Books — Anthony L. Komaroff, Harvard Medical School. “The Harvard Medical School Family Health Guide.” Simon and Schuster, 1999. ISBN: 9780684847030
- https://doi.org/10.1128/CMR.12.1.80 -- Fidel, Paul L., Jose A. Vazquez, and Jack D. Sobel. "Candida glabrata: review of epidemiology, pathogenesis, and clinical disease with comparison to C. albicans." Clinical Microbiology Reviews [12.1 (1999): 80-96].
- https://pubmed.ncbi.nlm.nih.gov/22041440/ -- Lin XL, Li Z, Zuo XL. "Study on the relationship between vaginal and intestinal candida in patients with vulvovaginal candidiasis." Chinese Journal of Obstetrics and Gynecology (Zhonghua fu chan ke za zhi). [2011 Jul;46(7):496].