See all "Discharge" Section Topics

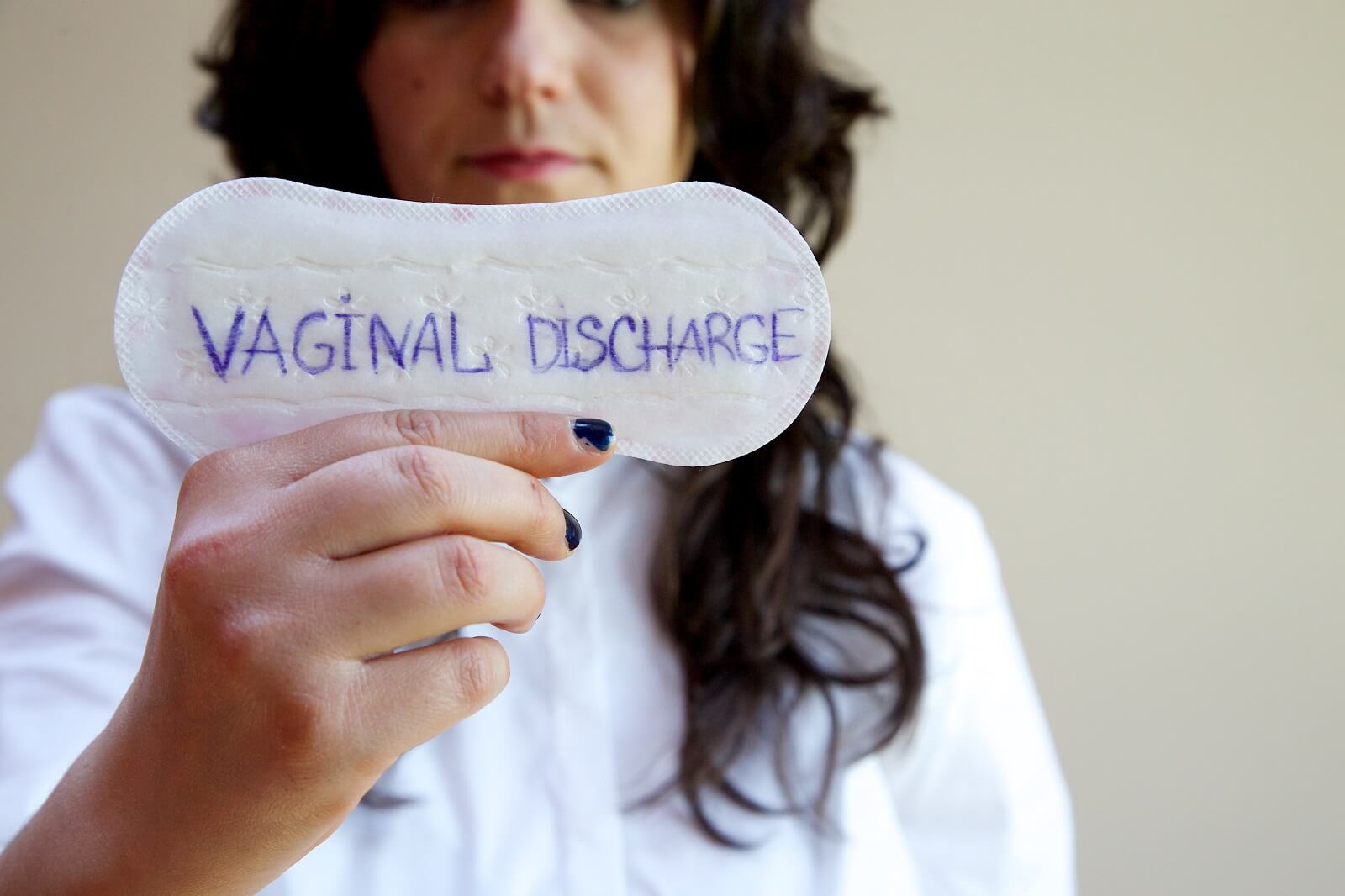
It is common that many women experience discharge that many have a strong odor to it, at times can smell fishy or an "amine" odor. This can happen cyclically or can be consistent.
If your discharge smells like fish, chances are you have the most common vaginal infection: bacterial vaginosis (BV). Bacterial vaginosis, which accounts for about 30% of vaginitis.
Some cases of BV are asymptomatic (no symptoms); and, in such instances, it is hard to even know you have this common bacterial infection.
The classical presentation of bacterial vaginosis is a triad of excessive vaginal discharge, frothy discharge and amine odor. A change in vaginal odor can also smell similar to fermentation or cheese like. For more information on this presentation of bacterial vaginosis please refer to the: Cheese Smelling Vaginal Discharge article.
Vaginal inflammation can be a symptom indicating that you do not have bacterial vaginosis or there is concomitant infection occurring.
Oral antibiotics often prescribed for bacterial vaginosis can often lead to vaginal candida overgrowth. Bacterial Vaginosis in conjunction with vaginal candida can often leads to inflammation of the vaginal tissue, otherwise knows as vaginitis.
Bacterial Vaginosis can greatly impact quality of life, but typically will not lead to inflammation of the vaginal tissue. Although antibiotics are typically prescribed for treatment of BV, reoccurence rates are high, up to 50-80% within a year of successful treatment.
And, as with many antibiotics treatments, typical side effects include candida overgrowth, which often times does not have an odor. However, severe yeast infections can lead to a yeasty, bread like smell. For more information you can check out: Yeast Infection Smell.
Unprotected sexual activity with multiple partners can lead to many kinds of sexually transmitted infections. Trichomoniasis, is a vaginal infection often mistaken for bacterial vaginosis. Bacterial vaginosis discharge can present from white to grey in color and is usually homogenous in texture. Trichomoniasis, has foul smelling odor that is not amine or yeast like, and often includes pain with urination and inflammation of the vaginal tissue.
So, if your vaginal discharge does not have a strong cheesy or fishy smell, and it is not white or a shade of grey, and you also are seeing inflammation of the vagina; trichomoniasis could be the cause of your bad vaginal odor and discharge.
A 1/2 Day & Yeast is Gone!
Linda Allen suffered from yeast infections for years. Through researching natural medicine & Candida, she found an efficacious solution!
Linda is one expert you want on your side! Let her show you how to get rid of a superficial yeast infection in just 12 hours; AND, keep it gone!
A 60-day, 100% money back guarantee is provided.
Visit Official Site!Bacterial Vaginosis Research
The first study we will examine, published in Genitourinary Medicine [68.2 (1992): 134], delineated the history and symptoms of BV quite thoroughly. The authors state that the nomenclature for BV has gone through many transitions; yet, it is commonly referred to simply as BV. Given the mild nature of this infection of the vagina, it was first considered to be “nonspecific vaginitis.”
The classically agreed upon symptoms for BV, have remained generally the same, since the condition’s discovery by medical science. The most noticeable; and classic sign of BV; is increased vaginal discharge with odor, and a strong vaginal odor. The smell caused by BV is nearly always “fishy;” although, it can have a “high cheese” smell in some cases.
This classic presentation, is commonly worse after sexual intercourse or menstruation. The discharge from the vagina is typically homogeneous, adheres to the vaginal wall in a thin film, and can range in color from white to a shade of grey. The authors state the condition is present in vaginas that have an elevated pH, and overgrowth of certain bacteria; most typically Gardnerella vaginalis.
According to the study, men can also develop an infection of the most common form of bacterial vaginosis, Gardernella Vaginalis. Yet, although the penis of males can become home to this bacteria; it has been difficult to prove this is a cause of initial BV or subsequent recurrent episodes of BV. Treating men with the prescription antibiotic metronidazole was not seen to reduce the recurrence of BV in women. A quote taken from the study explains this speculated relationship between infected men and women acquiring BV:
Gardner and Dukes also found that 90% of male sexual partners of women with BV were colonised with G. vaginalis suggesting that sexual transmission may occur and hence implying a causative role. Colonisation of the male urethra and semen has since been demonstrated but the association found by Gardner et al. with male sexual partners has proved difficult to reproduce. In addition treatment of the male partner with metronidazole has not decreased the recurrence rate of BV in women.
Genitourinary Medicine [68.2 (1992): 134]
Another study, published in the International Journal of Gynecology & Obstetrics [88.3 (2005): 281-285], outlines the basic signs and symptoms of BV. According to the authors, BV is the most common vaginal infection among women of reproductive age. The symptoms of BV include a foul, smelly vaginal discharge; and, in about half of the women who have BV, it can cause vaginal irritation. BV does not cause vaginal inflammation.
So, if you have a smelly, foul vaginal discharge, this is the hallmark symptom of BV. In a clinical study, the absence of a bad fishy smell and lack of excess vaginal discharge, were criteria for being cured of BV. After you get treated for BV, these symptoms should disappear.
The authors state that the cause of BV remains unknown; however, it happens when certain bacteria, primarily the anaerobic Gardnerella vaginalis, proliferate with a corresponding reduction of lactic acid producing bacteria. In women who visited clinics for sexually transmitted diseases, about 35% of them had BV. About 15 to 20% of pregnant women will contract BV; and, amongst women going to gynecologic clinics, 5 to 15% of them will be suffering from BV.
The Source of the Odor
The next study we will investigate, gives a solid explanation as to why BV causes a foul, fish odor. The study was published in APMIS [113.7?8 (2005): 513-516]. According to the study’s authors, trimethylamine (TMA) is an organic compound that can lead to the change in vaginal odor.
Human urine and fish muscle contain the non-volatile version of this chemical: trimethylamine oxide (TMAO) (Bystedt, et al.; 1959). When a fish dies, the bacteria in them, decompose the trimethylamine oxide into the odorous trimethylamine. When a woman has BV, the unwelcome bacteria in her vagina also reduce the trimethylamine oxide into the highly odorous trimethylamine. Hence, the vagina, and the discharge from it, exhibit a classic fishy smell.
Surprisingly, the study may reveal that eating fish can increase the fishy odor from urine and the vagina if you currently have BV. Although this postulation was not examined by the study, the research did state that by eating fish, you will have more TMAO in your body and vaginal fluid. Healthy young adults produce about 1 mg of TMA and 40 mg of TMAO daily; and, these levels can be drastically influenced by diet. When marine fish are included in the diet, several hundred mg of TMAO can be excreted by the body. Some individuals may not properly oxidize TMA; and, thus have less TMAO and more TMA in their vaginal secretions, urine, breath, and sweat—as a result of eating marine fish. The researchers found, on average, almost three times as much TMA in women with BV than women without BV. The study deduces that higher levels of TMA can therefore be a result of the bacteria causing BV reducing TMAO to TMA, a diet high in marine fish, and a possible rare physiological problem where the body cannot properly oxidize TMA. So, if you have BV, it is reasonable to assume eating fish can aggravate the foul vaginal smell.
Eliminate Bacterial Vaginosis & Vaginal Odor
Jennifer O’Brien is one prominent expert on BV that knows how to get rid of vaginal odor. BV is a common infection that you don’t have to put up with.
Jennifer will show you how to naturally eliminate vaginal odor in just 3 days.
A 60-day, 100% money back guarantee is provided.
Visit Official Site!Bacterial Vaginosis Recurrence
Another study also discusses recurrent BV and the prevalence of BV amongst women. The study was published in The Journal of Family Practice [60.2 (2011): 91]. According to the authors, BV is the most frequent cause of vaginal discharge; being responsible for up to 40 to 50% of clinical cases. Many medical professionals even state BV recurrence can be as high as 80% within a year after treatment. Among women aged 14 to 49 in the United States, BV currently affects about 30% of this population (asymptomatic cases included in this figure). The authors relate, that even with the use of the prescription drug metronidazole, recurrence frequently happens. According to an additional study, cited by the authors, there is up to a 50% chance a woman will redevelop BV within a year after successful treatment.
The authors also relate a study done on 120 Chinese women who had a history of BV (having two or more episodes in the previous year), but did not currently have it at the moment. The study found that women who used a probiotic pill were around half as likely, at various checkpoints in the future, to have BV—as compared to women who took a placebo alone. This shows some solid evidence that probiotic use can help stymie BV; and, help keep it from coming back.
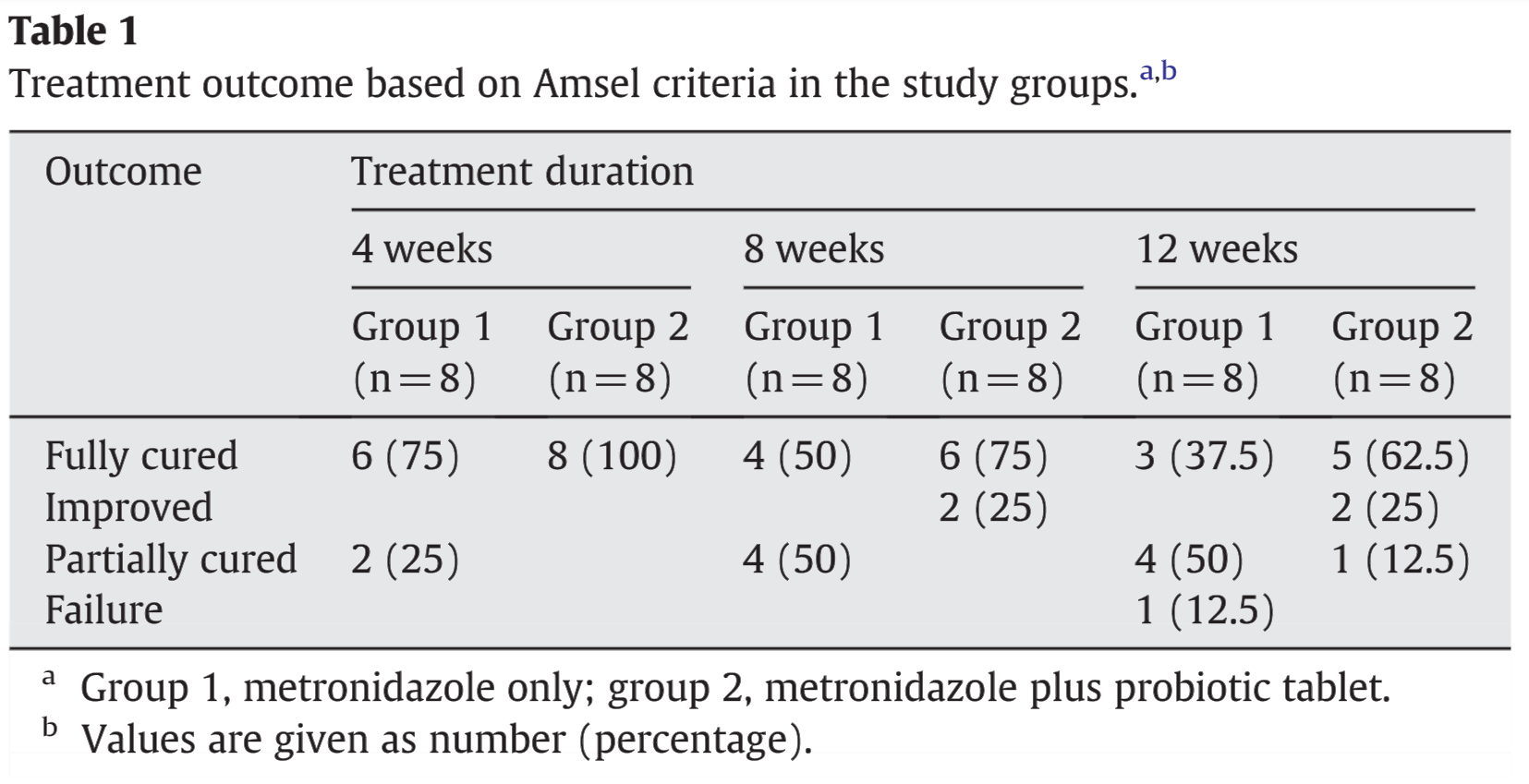
Since the rate of BV recurrence can be quite high; a method to help suppress BV more effectively was investigated in a study published in the International Journal of Gynecology & Obstetrics [108.3 (2010): 251-252]. The study took women who were suffering from recurrent BV (at least 3 different episodes in a year), who had failed to recover using 400 mg of oral metronidazole twice daily for 7 days, and divided them into two groups. The first group used a 0.75% metronidazole gel alone after menstruation; and, the second group used the metronidazole gel, plus they took a probiotic pill twice daily for three months. The study found that women who took a probiotic, in addition to using a vaginal metronidazole cream, had more success in keeping BV from recurring. The study used the Amsel criteria to diagnose BV. The following chart was taken from the study and illustrates the results of the experiment:
Clair Goodall: Author & Nature Lover
Clair Goodall is a bee-obsessed natural medicine convert from Minnesota. She is one expert you might want to know more about!
Clair will help you protect you and your family from toxic products and chemicals and help you discover solutions from nature.
Also, Clair’s book is backed by a 60-day, 100% money back guarantee
Visit Official Site!Trichomoniasis: Another Cause of Vaginal Odor
According to the 2014 edition of The Gale Encyclopedia of Alternative Medicine, trichomoniasis can also cause unusual vaginal odor and discharge. Like yeast infections, the use of antibiotics can increase a woman’s likelihood for contracting the protozoan that causes trichomoniasis. The text states, that the symptoms of trichomoniasis in women, include the following:
- A foul, smelly vaginal odor.
- Profuse, yellow, frothy vaginal discharge.
- Intense itching of the vaginal area.
- Inflammation and irritation of the labia, vagina, or cervix.
- Pain during urination (dysuria).
- Pain during sexual intercourse (dyspareunia).
- Women may sometimes have lower abdominal pain.
So, if you have a yellow or green vaginal discharge, you have vaginal inflammation, and do not have a “cheesy” or “fishy” vaginal odor, you may have trichomoniasis instead. But, since trichomoniasis is an STD, you can probably rule such a malady out completely, if you haven’t had sexual activity that could put you at risk. Also, BV can occur along with other vaginal problems, so if you have a classic BV associated vaginal smell and vaginal inflammation (or another classic symptom of Candidiasis or trichomoniasis), you probably have more than one vaginal infection!
The Big 3 Vaginal Infections
Yeast infections, BV, and trichomoniasis are three massively widespread vaginal infections. If you have a strange odor, and none of the other symptoms of vaginal Candidiasis, you can probably rule out completely that you have this infection. But, again, BV and trichomoniasis can resemble each other to some degree—due to both causing fishy, foul vaginal odor.
In a study published in The Female Patient [22 (1997): 39-56], the multiple medical researchers involved, stated millions of American women received prescriptions for some form of vaginitis (vaginitis is any type of vaginal infection). Of the women who will come down with some vaginal infection, BV is the most prevalent; accounting for about 45% of all vaginitis cases. Yeast infections came in second, causing about 40% of all vaginal infections.
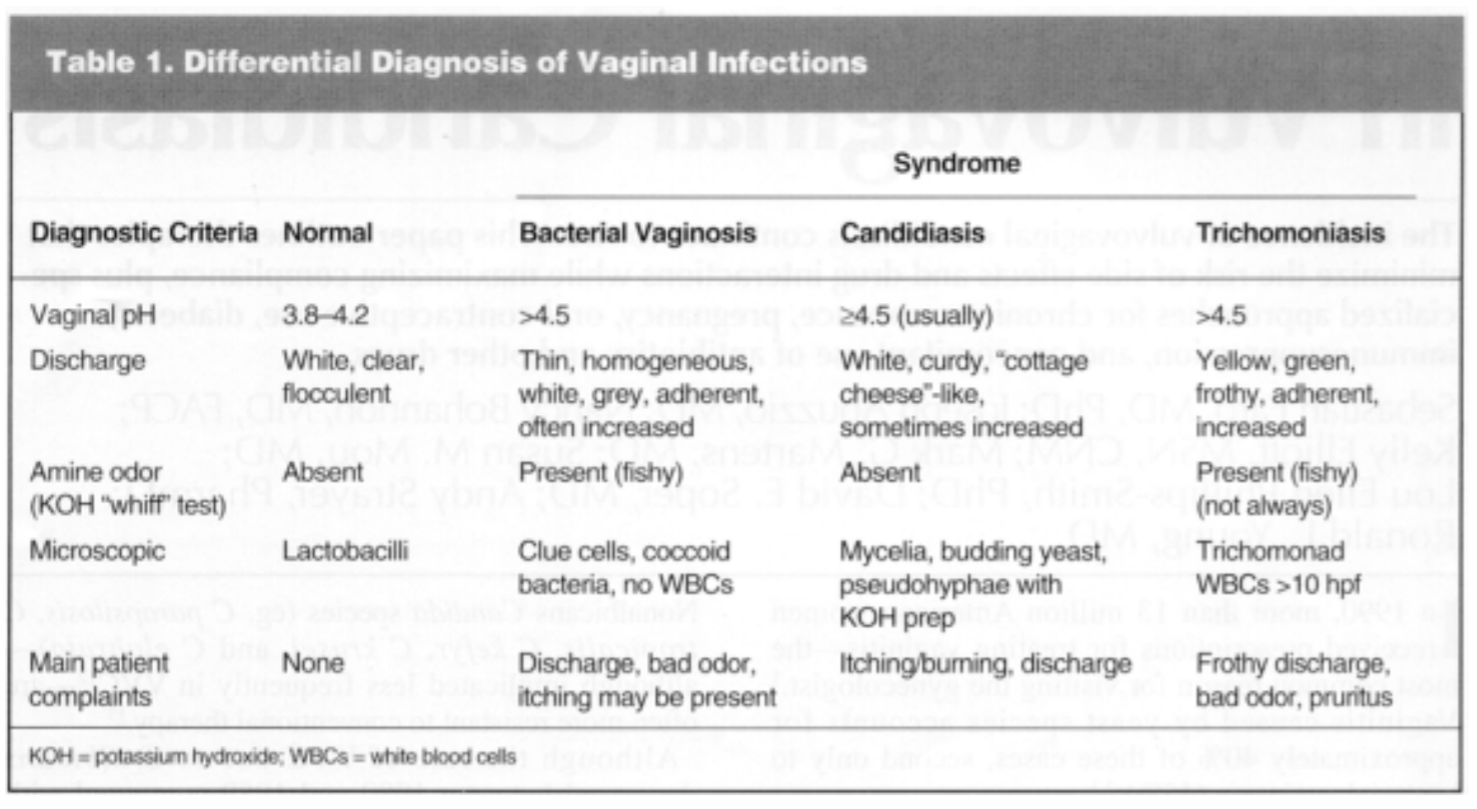
Trichomoniasis, isn't as common of an infection as BV or vaginal candidiasis. The following chart, was taken from the study, and shows you how to differentiate between these infections. Vaginal odor (as noted by the “amine odor”; remember trimethylAMINE), vaginal pH, discharge, and chief complaints women have with these conditions, are delineated in the chart. Note the discharge color difference between BV and trichomoniasis; this may be essential to helping you rule out trichomoniasis.
Linda Allen’s 12 Hour Yeast Infection Treatment

A significant portion of women will end up suffering from recurrent vaginal yeast infections. You may even be a victim of this tragic condition yourself. One woman, Linda Allen, ended up having recurrent yeast infections early in her life. And, for about a decade thereafter, Candida would rob her of her health and well being.
Linda’s yeast related health problems started in her late teen years; about the same time she developed a sinus infections. It was around this time that Linda came down with a vaginal yeast infection. Linda wasted little time before she consulted a doctor for help. The physician quickly wrote out a prescription for her. Linda found that using this antifungal drug, her yeast infection cleared up rapidly; and, her problem appeared to be over. But, after time passed, Linda found she had developed another yeast infection. Again, Linda went back to her doctor and got another prescription. The yeast infection again went away. Yet, it did not stay gone long; after a short while, Linda found herself infected again by Candida.
The cycle of yeast infection recurrence would last about a decade in Linda’s life. All the while Linda dealt with outward yeast infections, her general health continued to worsen. She spent a small fortune on prescription drugs and medical bills. Doctors would prescribe her stronger and stronger antibiotics to deal with the myriad of problems she was having. And, she was even put on allergy medications to help relieve her symptoms. Yet, these drugs only improved her condition temporarily; they never offered her a complete, permanent solution. Those who knew Linda began to wonder if she was just sicker than she was letting on; or, perhaps she was a little bit of a hypochondriac. All of Linda’s medical bills began to add up; she could have bought her first house with the money she put into fixing her health!
Linda’s life did change for the better one fateful day, when she decided to visit a naturopath about her health. The naturopath knew exactly what was going on with Linda’s body and told her she was suffering from systemic yeast overgrowth. The naturopath was not able to totally end Linda’s yeast problems; but, it was a revelation that gave her a starting point to go from.
Linda began to become very interested in holistic, natural medicine. She bought a host of medical books and spent an extended amount of time studying them. When Linda found a doctor or medical expert willing to lend her some time, she consulted them for advice. Linda tried a wide array of alternative methods for curing Candida; and, although none worked totally, they occasionally provide her with key insights.
Eventually, Linda began to correlate her experience with these natural treatments and applied her knowledge of Candida to arrive at a powerful treatment plan. Linda spent a year polishing and perfecting her new approach. The time finally came when Linda applied her new approach to herself. Linda found that she began to rapidly improve after starting this new therapy. Her vaginal yeast infections went away; and, as time went on, her health improvements did not dissipate. Eventually Linda felt like her old, healthy self again! Linda gave others her new method and they too found that all their symptoms would melt away quickly using her therapy. Linda had finally arrived at a permanent, safe, and natural cure for her Candida problem.
Linda has since published a book detailing her entire Candida treatment program. Linda guarantees that oral and genital yeast infections will be totally cured in just 12 hours time using the method outlined in her book. And, after a few weeks have passed; even stubborn, systemic Candida overgrowth will be eradicated from the body! Since Linda’s book was published in 2004, over 100,000 individuals from around the world have seen amazing results using Linda’s treatment.
Linda Allen’s book is published by a large, reputable online retailer—which is owned by the U.S. based firm Keynetics Incorporated. Linda’s publisher has been doing business since nearly the advent of the internet; and, you can be assured of a safe, easy purchase. And, Linda guarantees her her 12 hour cure time for oral and genital yeast infections; if they don’t go away in half a day, you can get all your money back by making a quick request to Linda’s publisher. Linda’s book is available as a digital ebook you can download instantly if you decide to give it a try! There is no need to return anything if you request a refund.
To learn a bit more about Linda’s personal story and journey to better health, to see testimonials from many happy people who tried Linda’s book, or to see some of the free bonus books she offers with her’s, you can find out more information any time at Linda Allen’s website.
Author: Mr. Nicholas Gross

Nick Gross is a natural medicine enthusiast who has been researching and writing about natural medicine since 2008. Nick is primarily a web developer but also researches and authors written and video content about natural health. Nick has a bachelor’s degree in Management Information Systems from the University of Northern Iowa.
Disclaimer
The information on this website is not a prescription for anyone. This information is for informational or educational purposes only, and is not a substitute for professional medical advice or consultations with healthcare professionals.
Affiliate Disclosure
Some of the links provided on this website are affiliate links. When a purchase is made through these links, Candida Hub earns money from commission. This helps to keep the website up and helpful to people for free. Thank you for any support!
Stay Up to Date
If you enjoyed this article, consider following / liking our Facebook page. This page is primarily utilized to alert followers of new articles that are put on Candida Hub. Candida related news is also discussed. While you are there, you can see what has been more recently added to Candida Hub.
SOURCES:
- http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1194827/ — Easmon, C. S., P. E. Hay, and C. A. Ison. "Bacterial vaginosis: a diagnostic approach." Genitourinary medicine 68.2 (1992): 134. PubMed PDF
- http://dx.doi.org/10.1016/j.ijgo.2004.11.028 — Núñez, J. T., and G. Gómez. "Low-dose secnidazole in the treatment of bacterial vaginosis." International Journal of Gynecology & Obstetrics 88.3 (2005): 281-285. PubMed
- http://dx.doi.org/10.1111/j.1600-0463.2005.apm_175.x — Wolrath, Helen, et al. "Trimethylamine and trimethylamine oxide levels in normal women and women with bacterial vaginosis reflect a local metabolism in vaginal secretion as compared to urine." Apmis 113.7?8 (2005): 513-516. PubMed
- http://dx.doi.org/10.1002/jsfa.2740100601 — Bystedt, J., L. Swenne, and H. W. Aas. "Determination of trimethylamine oxide in fish muscle." Journal of the Science of Food and Agriculture 10.6 (1959): 301-304.
- http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3183959/ — Jones, Kohar, and Bernard Ewigman. "Help for recurrent bacterial vaginosis." The Journal of family practice 60.2 (2011): 91.
- http://dx.doi.org/10.1016/j.ijgo.2009.09.029 — Thulkar, Jyoti, Alka Kriplani, and Nutan Agarwal. "Probiotic and metronidazole treatment for recurrent bacterial vaginosis." International Journal of Gynecology & Obstetrics 108.3 (2010): 251-252. PubMed
- Google Books — The Gale Encyclopedia of Alternative Medicine Ed. Laurie J. Fundukian. Vol. 4. 4th ed. Farmington Hills, MI: Gale, 2014. p2433-2435. COPYRIGHT 2014 Gale, Cengage Learning
- https://www.researchgate.net/publication/242115516 — Young, Ronald L. "Treatment considerations in vulvovaginal candidiasis." The Female Patient 22 (1997): 39-56.PDF Available Here








