See all "Answers" Section Topics

According to the vast amount of research on Candida infections of the skin and hair follicles, the relating of hair loss as a symptom of this condition, is rare or possibly non-existent. There is little evidence available that suggests hair loss is related to Candida overgrowth alone.
Yet, if you are having intense, repeat yeast infections; and, you started to loose your hair, you may have a genetic disorder. Chronic mucocutaneous Candidiasis is a genetic disorder in which the t-cells lack the ability to properly defend against specific pathogens—most commonly Candida.
Some individuals with this genetic disorder, about half of them, also have an endocrine problem. This disruption in the hormone producing glands of the body leads to excessive alopecia (hair loss).
As research suggests, incidences where the hair follicles become infected with Candida, do not seem to cause hair to fall out. Research in this area does seem to be lacking; so, it could be possible that you are truly losing hair due to the single influence of Candida.
Yet, this is perhaps very rare; and, you likely have a genetic condition that is causing your endocrine system to perform abnormally. Also, as you will see, antifungal drugs can routinely cause hair loss; thus, it would appear that your yeast infection is not the source of this problem—if you are taking these drugs.
So, Candida causing hair loss, by itself, is perhaps extremely rare; if it even happens at all.
A 1/2 Day & Yeast is Gone!
Linda Allen suffered from yeast infections for years. Through researching natural medicine & Candida, she found an efficacious solution!
Linda is one expert you want on your side! Let her show you how to get rid of a superficial yeast infection in just 12 hours; AND, keep it gone!
A 60-day, 100% money back guarantee is provided.
Visit Official Site!Candida & Hair Loss Research
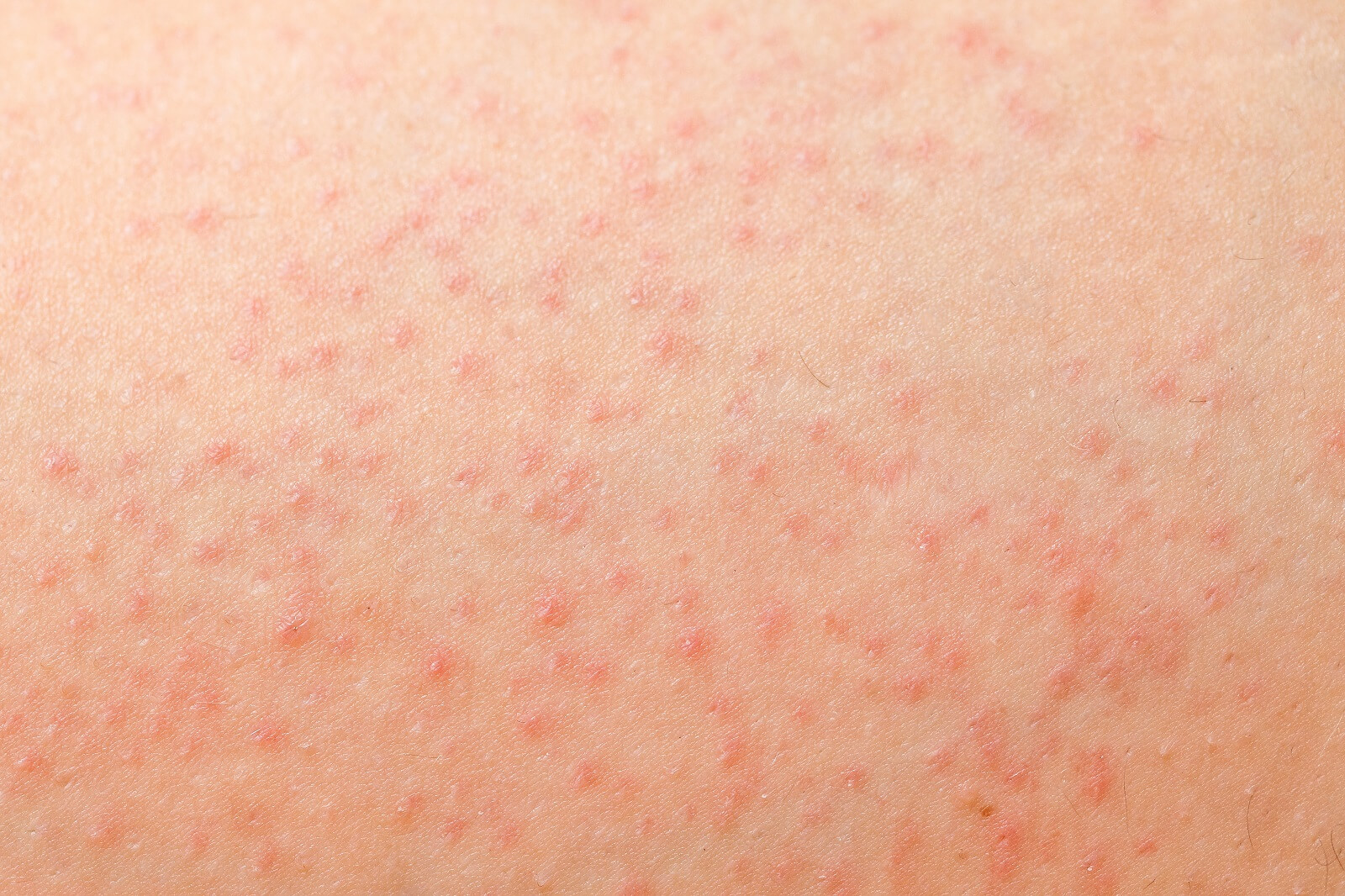
A 2014 study, published in the Journal of Correctional Health Care [20.2 (2014): 154-162], related the story of a prison that had around 35 male inmates suffering from Candida infections on their skin. Five of these affected men, were brought into a clinic for evaluation.
The study relates the story of these five inmates’ Candida problems. All of them had some form of folliculitis; 3 of the five likely had Malassezia folliculitis, while the other two were positive for Candida albicans induced folliculitis. In the cases of these men who had yeast infections of the skin and hair follicles, nothing was reported about hair loss. So this research suggests that hair loss is a very uncommon symptom of Candida overgrowth.
Another study, published in Mycoses [55.2 (2012): e20-e22], reported the case of a man who had Candida colonizing his beard (this study was addressed above, with the image of the man displayed). The affected man was diagnosed with Candida folliculitis.
In the case report, present in the study describing the man’s condition, nothing was mentioned about this man having a loss of facial hair due to the folliculitis attacking his beard. The man related that he had engaged in oral sexual activity right before he developed the infection around his mouth. The study stated that this sexual contact was a likely instigator of the Candida folliculitis infection—as Candida can readily pass from genitals or oral cavities colonized by the yeast.
Therefore, this is another study that suggests Candida, even when it colonizes hair follicles, does not usually cause hair loss. The following quotation was taken from the study, and relates information regarding Candida folliculitis and the likely health maladies that can predispose someone to such an infection.
Candida folliculitis (CF) is predominantly limited to hair follicles of beard and moustache area in men, and less frequently to the scalp. In addition to abovementioned predisposing factors for Candida infections, Candida colonisation of the mouth, or the mouth of the partner, and an infected razor have been suggested for the development of CF. There are reports of CF occurring in patients with hypothyroidism, agranulocytosis, malignant tumours and immunode?ciency syndromes.
http://dx.doi.org/10.1111/j.1439-0507.2011.02075.x

Another study, published in Mycoses [1999; 42(11-12):683-5], relates the case of a man who had folliculitis barbae (an infection of hair follicles of the beard) due to Candida albicans. The researchers reported that the man had inflamed reddened skin around his mouth and nose, and the area was painful and filled with pus filled bumps.
Yet, in all the discussion about the symptoms this man had, nothing was reported about hair loss. Thus, it is again seen that this study relating the case of a hair follicle Candida infection, does not suggest that the loss of hair is common to this condition.
In some rare instances, untreated Candida folliculitis may cause hair loss. Hair follicle infection known to cause hair loss is folliculitis decalvans (a rare inflammation of the scalp which commonly presents as painful hair follicles that also ooze pus). According to a study, published in the International Journal of Trichology [2.1 (2010): 20], folliculitis decalvans can lead to hair loss.
The cause of this condition is relatively elusive and unknown. There have been attempts to use antifungals to treat this condition. Consequently, some form of Candida may be responsible for such severe infection of the hair follicle.
Eliminate Bacterial Vaginosis & Vaginal Odor
Jennifer O’Brien is one prominent expert on BV that knows how to get rid of vaginal odor. BV is a common infection that you don’t have to put up with.
Jennifer will show you how to naturally eliminate vaginal odor in just 3 days.
A 60-day, 100% money back guarantee is provided.
Visit Official Site!Antifungals and Hair Loss
A study, published in the Annals of Pharmacotherapy [2014], relates the story of a 34 year old woman who noticed hair loss after she began taking anidulafungin at a dose of 100 mg per day. After being on this prescription antifungal for one month, the woman noticed significantly greater hair loss than usual.
After 3 months of using the drug, the patient stopped taking the drug as she was noticing it was very easy to pull out her hair, had more hair loss, and began to develop alopecia plaques of 1 to 2 cm in size. After terminating the anidulafungin regimen, the hair loss stopped.
Other azole antifungal drugs have been known to cause hair loss as well. The study stated alopecia is a common side effect of voriconazole, a rare side effect of fluconazole and ketoconazole, and an uncommon side effect of itraconazole.
Thus, given the wide breadth of azole drugs that can cause hair loss, this condition may be due to one of these drugs. The possible relation between your Candida infection and your hair loss would then be a spurious correlation—the true cause being the antifungal you're using.
Another more comprehensive study, that looked at hair loss caused by fluconazole, was published in the Annals of Internal Medicine [123.5 (1995): 354-357]. The study found that 17 of a group of 136 patients on fluconazole—about 12.5%—had hair loss. In another group of 40 patients on fluconazole, 8 (20%) had hair loss. Many of the patients in the study were on high doses of fluconazole; some received 400 mg daily for an average of about 7 months.
Hair loss, on average, started after 3 months of the fluconazole treatment regimen. The scalp area was affected in all of those who had hair loss; one third of the patients also had hair loss on other areas of their bodies. The hair loss caused by this drug resolved within 6 months since discontinuation of fluconazole or reducing the dosage by a minimum of 50%.
The concluding remarks of the researchers stated the following about alopecia induced by fluconazole:
In summary, substantial alopecia appears to be much more commonly associated with fluconazole than was previously recognized, particularly when the drug is given at larger doses (400 mg / day) and for prolonged periods (2 months). The pattern of hair loss almost always involves the scalp and may involve other sites. The alopecia reverses with discontinuation of fluconazole therapy or dose reduction. This adverse event does not appear to be linked to other toxicities, such as liver function abnormalities, impotence, or gastrointestinal disturbances.
http://dx.doi.org/10.7326/0003-4819-123-5-199509010-00006
One of the only studies that seems to be available relating the association between Candidal folliculitis and hair loss was published in Laboratory Animal Research [27.1 (2011): 63-65]. There is an important caveat however: the subject with the Candida problem was a dog! The dog had a skin infection, hair loss, and scaly skin.
There were no parasites detected on the dog; but, Candida was successfully found in the dog’s lesions. The researchers concluded, that Candida could be a cause of the alopecia in the dog. This study was published in 2011; and, the researchers said that as far as they knew, this was the first case of Candida causing these problems in dogs they were aware of.
Clair Goodall: Author & Nature Lover
Clair Goodall is a bee-obsessed natural medicine convert from Minnesota. She is one expert you might want to know more about!
Clair will help you protect you and your family from toxic products and chemicals and help you discover solutions from nature.
Also, Clair’s book is backed by a 60-day, 100% money back guarantee
Visit Official Site!Chronic Mucocutaneous Candidiasis
A study, published in the Annals of Internal Medicine [89.1 (1978): 91-106], also reiterated the fact that hair loss can be due to a genetic disorder that leads to the condition chronic mucocutaneous Candidiasis.
If you seem to always be plagued by chronic Candida infection of the skin, nails, hair, or mucous membranes (such as in the mouth or vagina), and your also noticing hair loss, it is possible you could have chronic mucocutaneous candidiasis.
Chronic mucocutaneous candidiasis is a genetic problem in which the T-cells do not function correctly and are unable to adequately protect the body from Candida. The sign of hair loss, along with chronic yeast infections, is a solid indicator you indeed have this genetic problem; as hair loss is not a normal side effect of Candida overgrowth, but does frequently occur in individuals with this genetic problem.
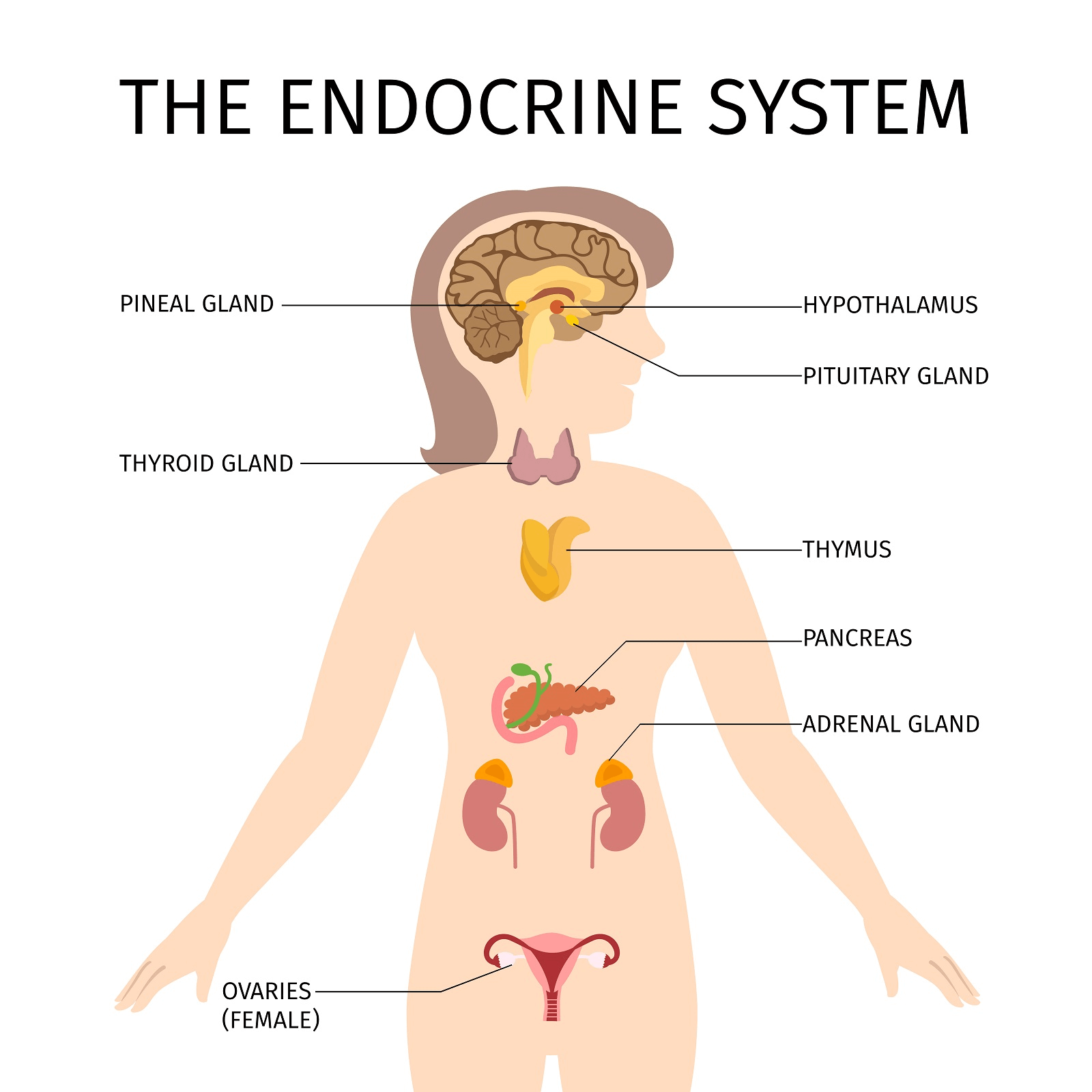
The study stated that in about half of all those with this genetic trait, endocrine abnormalities will occur. The endocrine system is comprised of various glands that create hormones; thus, hormonal problems can result from disruption of the endocrine system’s functions.
Hypoparathyroidism, Addison's disease, and less commonly hypothyroidism and diabetes, will occur. Severe hair loss can start, and continue to occur, in those individuals that have this problem. Although some claim that the toxins created by Candida are responsible for thyroid dysfunction and hair loss; this may indeed be a spurious association—the real cause being the genetic malfunction.
A Natural, 12 Hour Yeast Infection Cure

According to a research paper published in Clinical Microbiology Reviews [12.1 (1999): 80-96], Candida species are quite ubiquitous organisms. Candida are most frequently present in the mouth; and, live in 31% to 55% of healthy people. The species that causes approximately 70% to 80% of all Candida infections is C. albicans.
The Chinese Journal of Obstetrics and Gynecology [2011 Jul;46(7):496] reports there appears to be a correlation between intestinal Candida infections and vaginal yeast infections. And, this provides a clue, as to why yeast infections in general, can reoccur.
This study states, in 148 cases of vaginal candida infections, 33.1% of the women were infected in both the intestines and vaginal area. The recurrence rate of yeast infections, in women with simultaneous intestinal infection, was significantly higher than for women who did not have an intestinal infection. This study concluded that vaginal yeast infections are highly associated with simultaneous intestinal Candida infection.
As research appears to indicate, systemic Candida infections can and do happen. A more systemic Candida infection may primarily get a foothold in the intestines; and cause a wide array of problems. If your yeast infections keep happening, a systemic Candida problem may be why.
One woman who suffered from a systemic Candida infection, for about 12 years, was Linda Allen. The systemic Candida infection that attacked Linda caused a wide range of health problems in addition to yeast infections. Some of these problems, Linda describes in her own words in the following quote:
To be honest, it was hard to pinpoint exactly what was wrong: I wasn’t really sick, but I wasn’t really well either. I had listlessness, fatigue, brain fog, stomach ailments, unexplained rashes, skin infections, and so on. It seemed like every day brought a new challenge.
My energy was sapped and I felt exhausted, which affected my grades and put a big dent in my social life.
Linda Allen’s symptoms included an embarrassing vaginal discharge, severe itching, and burning sensations. Her infections were difficult to deal with, and Linda’s health problems cost her financially as well. Linda states these infections of Candida can become excruciating when they happen as frequently as a menstrual period.
Yet, Linda spent a great deal of time in research; and even questioned health professionals who were kind enough to share some time with her. Linda even tried an array of purported "cures." Although it took a while, eventually, Linda put together a natural treatment plan she hoped would solve her Candida situation.
After spending about a year refining her new approach, Linda tried her system on herself. It worked amazingly well. Linda even returned to a few medical doctors to get tested for the presence of infections. These tests revealed all indicators of infection had vanished! Linda was indeed well again, after such a long, difficult journey.
Linda has since published a book detailing how to copy her success. She also includes a 12 hour yeast infection cure that can get rid of a superficial (such as a genital yeast infection or oral thrush) yeast infection in about 12 hours.
Linda’s publisher protects those who get her book with a 60 day, 100% money back guarantee. Linda’s publisher, a subsidiary of the United States based firm Keynetics Incorporated, is a reputable digital retailer that has been around for a long time.
They have great customer service, and make getting a full refund on Linda’s book quick and easy. If you’re not satisfied, you can quickly get all your money back.
If you would like to learn more about Linda’s journey to freedom from Candida, see reviews of others who tried her natural system, or find out more about her efficacious book; you can find more information at Linda Allen’s website.
Author: Mr. Nicholas Gross

Nick Gross is a natural medicine enthusiast who has been researching and writing about natural medicine since 2008. Nick is primarily a web developer but also researches and authors written and video content about natural health. Nick has a bachelor’s degree in Management Information Systems from the University of Northern Iowa.
Disclaimer
The information on this website is not a prescription for anyone. This information is for informational or educational purposes only, and is not a substitute for professional medical advice or consultations with healthcare professionals.
Affiliate Disclosure
Some of the links provided on this website are affiliate links. When a purchase is made through these links, Candida Hub earns money from commission. This helps to keep the website up and helpful to people for free. Thank you for any support!
Stay Up to Date
If you enjoyed this article, consider following / liking our Facebook page. This page is primarily utilized to alert followers of new articles that are put on Candida Hub. Candida related news is also discussed. While you are there, you can see what has been more recently added to Candida Hub.
SOURCES:
- http://dx.doi.org/10.1177/1078345813518636 — Jalalat, Sheila, et al. "An outbreak of Candida albicans folliculitis masquerading as Malassezia folliculitis in a prison population." Journal of Correctional Health Care 20.2 (2014): 154-162. PubMed
- http://dx.doi.org/10.1111/j.1439-0507.2011.02075.x — Mansur, Ayse Tülin, Ikbal Esen Aydingoz, and Seza Artunkal. "Facial Candida folliculitis: possible role of sexual contact." Mycoses 55.2 (2012): e20-e22. PubMed
- http://dx.doi.org/10.1046/j.1439-0507.1999.00531.x — Süß, Katrin, Irina Vennewald, and C. Seebacher. "Case report. Folliculitis barbae caused by Candida albicans." Mycoses 1999; 42(11-12):683-5. PubMed
- http://dx.doi.org/10.4103%2F0974-7753.66908 — Sillani, Caulloo, et al. " Effective treatment of folliculitis decalvans using selected antimicrobial agents." International journal of trichology 2.1 (2010): 20. PubMed Full Text
- http://dx.doi.org/10.1177/1060028014524534 — Ruiz-Ramos, J., et al. " Anidulafungin-induced alopecia." Annals of Pharmacotherapy (2014): 1060028014524534. PubMed
- http://dx.doi.org/10.7326/0003-4819-123-5-199509010-00006 — Pappas, Peter G., et al. "Alopecia associated with fluconazole therapy." Annals of internal medicine 123.5 (1995): 354-357. PubMed
- http://dx.doi.org/10.5625%2Flar.2011.27.1.63 — Lee, Hyun-A., et al. "Mural folliculitis and alopecia with cutaneous candidiasis in a beagle dog." Laboratory animal research 27.1 (2011): 63-65. PubMed Full Text
- http://dx.doi.org/10.7326/0003-4819-89-1-91 — EDWARDS, JOHN E., et al. "Severe candidal infections: clinical perspective, immune defense mechanisms, and current concepts of therapy." Annals of internal medicine 89.1 (1978): 91-106. PubMed
- https://doi.org/10.1128/CMR.12.1.80 -- Fidel, Paul L., Jose A. Vazquez, and Jack D. Sobel. "Candida glabrata: review of epidemiology, pathogenesis, and clinical disease with comparison to C. albicans." Clinical Microbiology Reviews [12.1 (1999): 80-96].
- https://pubmed.ncbi.nlm.nih.gov/22041440/ -- Lin XL, Li Z, Zuo XL. "Study on the relationship between vaginal and intestinal candida in patients with vulvovaginal candidiasis." Chinese Journal of Obstetrics and Gynecology (Zhonghua fu chan ke za zhi). [2011 Jul;46(7):496].