See all "Candida Odor" Section Topics

Are you unsure if you have a yeast infection or bacterial vaginosis? If you are experiencing symptoms of both, you might even have both types of infection. Bacterial vaginosis is caused by an overgrowth of pathogenic bacteria in the vagina. Yeast infections are caused by the overgrowth of a yeast in the Candida genus; typically Candida albicans. It is likely you have either one or the other vaginal malady; however, since both can be present in the vagina simultaneously, you might have both.
One telltale sign of a yeast infection, are creamy, white lesions in the vagina or affected area. These lesions often bleed slightly if scraped away. If you're not noticing any “fishy” odor coming from the vagina or from vaginal discharge, you likely have just a yeast infection. The discharge caused by a yeast infection, if present, will look like cottage cheese and possibly have a “yeasty” odor similar to beer or bread. Typically, irritation and itching, will nearly always be present as well. Conversely, if you do not see any white lesions in the vagina or have cottage cheese like vaginal discharge; and, don’t have any genital itching, you you may not have a yeast infection.
If you don’t have the signs of a Candida problem, but do have a thin, greyish vaginal discharge; and, have a foul, fishy smelling vagina; you likely have bacterial vaginosis. Itching can also accompany bacterial vaginosis, as well; so, itching not a great indicator of what type of infection you have.
A 1/2 Day & Yeast is Gone!
Linda Allen suffered from yeast infections for years. Through researching natural medicine & Candida, she found an efficacious solution!
Linda is one expert you want on your side! Let her show you how to get rid of a superficial yeast infection in just 12 hours; AND, keep it gone!
A 60-day, 100% money back guarantee is provided.
Visit Official Site!Vaginal Infection Research
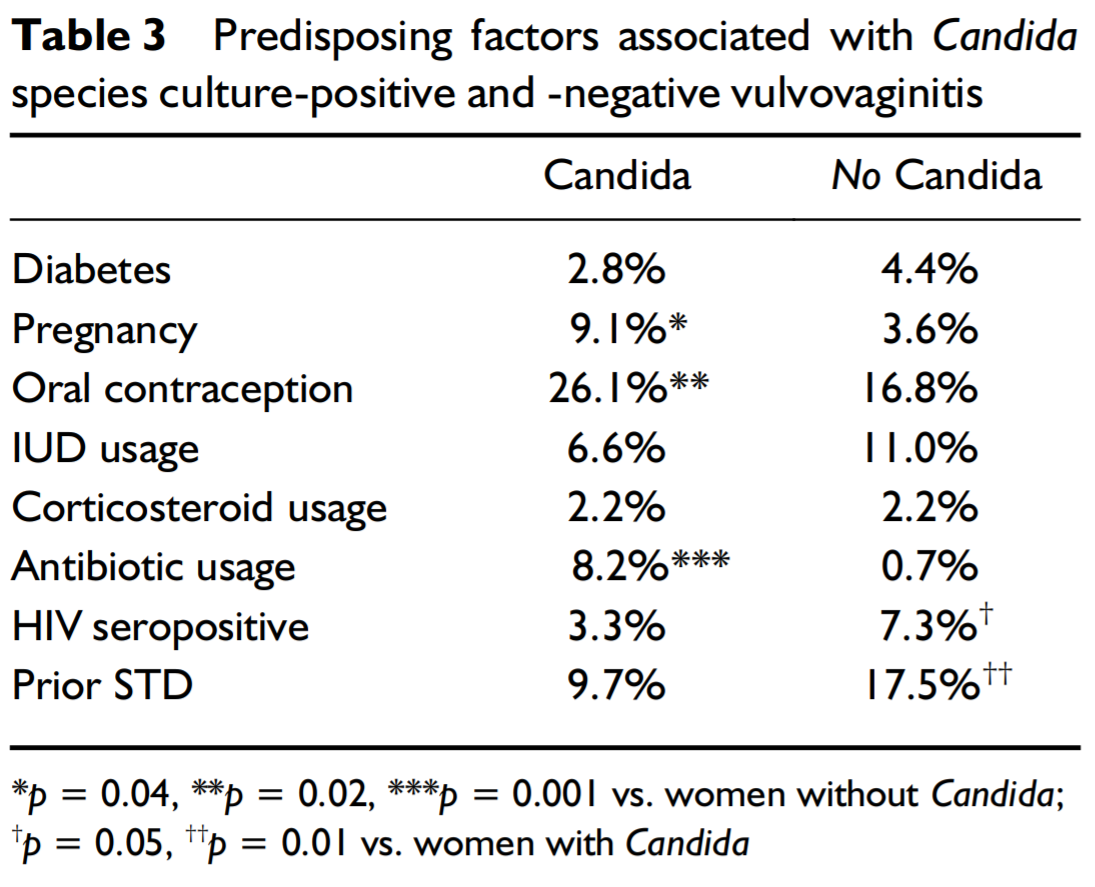
One study was fairly comprehensive, in that it analyzed 501 women who complained of vaginal discharge or itching in the vaginal area. The study was published in Infectious Diseases in Obstetrics and Gynecology [2001; 9:221–225]. These women were screened to see if they indeed had a yeast infection. Of the 501 women, about 73% were positive for Candida; over 80% of Candida positive women had Candida albicans. This suggests that if you do have a vaginal discharge, or experience uncommon vaginal itching, you likely have a yeast infection. Factors that were correlated to the presence of Candida, were antibiotic use and the use of oral contraceptives. If you have taken either of these forms of medication, you are more likely to have Candida; and not bacterial vaginosis.
The chart below, was taken from this study in Infectious Diseases in Obstetrics and Gynecology. The chart shows how various factors predisposed women to being positive for a vaginal Candida infection. The “p,” referred to by the lower part of the chart, shows the accuracy, in terms of probability, of the statistics presented.
Eliminate Bacterial Vaginosis & Vaginal Odor
Jennifer O’Brien is one prominent expert on BV that knows how to get rid of vaginal odor. BV is a common infection that you don’t have to put up with.
Jennifer will show you how to naturally eliminate vaginal odor in just 3 days.
A 60-day, 100% money back guarantee is provided.
Visit Official Site!Candida, Trichomonas vaginalis, and Gardnerella vaginalis
Another study, shows how difficult it can be to differentiate between three common types of vaginal infection: yeast infection (Candida species), Trichomoniasis (Trichomonas vaginalis), and bacterial vaginosis (Gardnerella vaginalis). The study was published in Health SA Gesondheid [6.1 (2001): 21-27]. The study utilized 70 different pregnant women who had a vaginal infection of some kind. The study evaluated how well a clinic could initially diagnose these women using a medical history exam and pictures of various vaginal infections. Surprisingly, the clinic misdiagnosed the infections quite frequently. This indicates, that mild types of infections without direct symptoms, can be difficult—even for professionals—to diagnose.
Given the inaccuracy, demonstrated by clinical professionals, it is possible that you could misdiagnose yourself. Common vaginal infections often present similar signs and symptoms; and, it is hard for professionals to know for sure without laboratory findings. There is a more efficacious way to be more certain your problems are being caused by yeast. Candida Hub has adapted a test developed by the late Dr. William Crook; an expert on the topic of yeast and how it influences the health of individuals. There is a short version of this test if you don’t have too much time to invest; and, a long version of this test that can give a more comprehensive assessment. Remember, Candida can live in your digestive system and have far more negative effects on you than just a vaginal infection. To check out these tests visit this page: Home Yeast Infection Tests.
Clair Goodall: Author & Nature Lover
Clair Goodall is a bee-obsessed natural medicine convert from Minnesota. She is one expert you might want to know more about!
Clair will help you protect you and your family from toxic products and chemicals and help you discover solutions from nature.
Also, Clair’s book is backed by a 60-day, 100% money back guarantee
Visit Official Site!Bacterial Vaginosis Symptoms
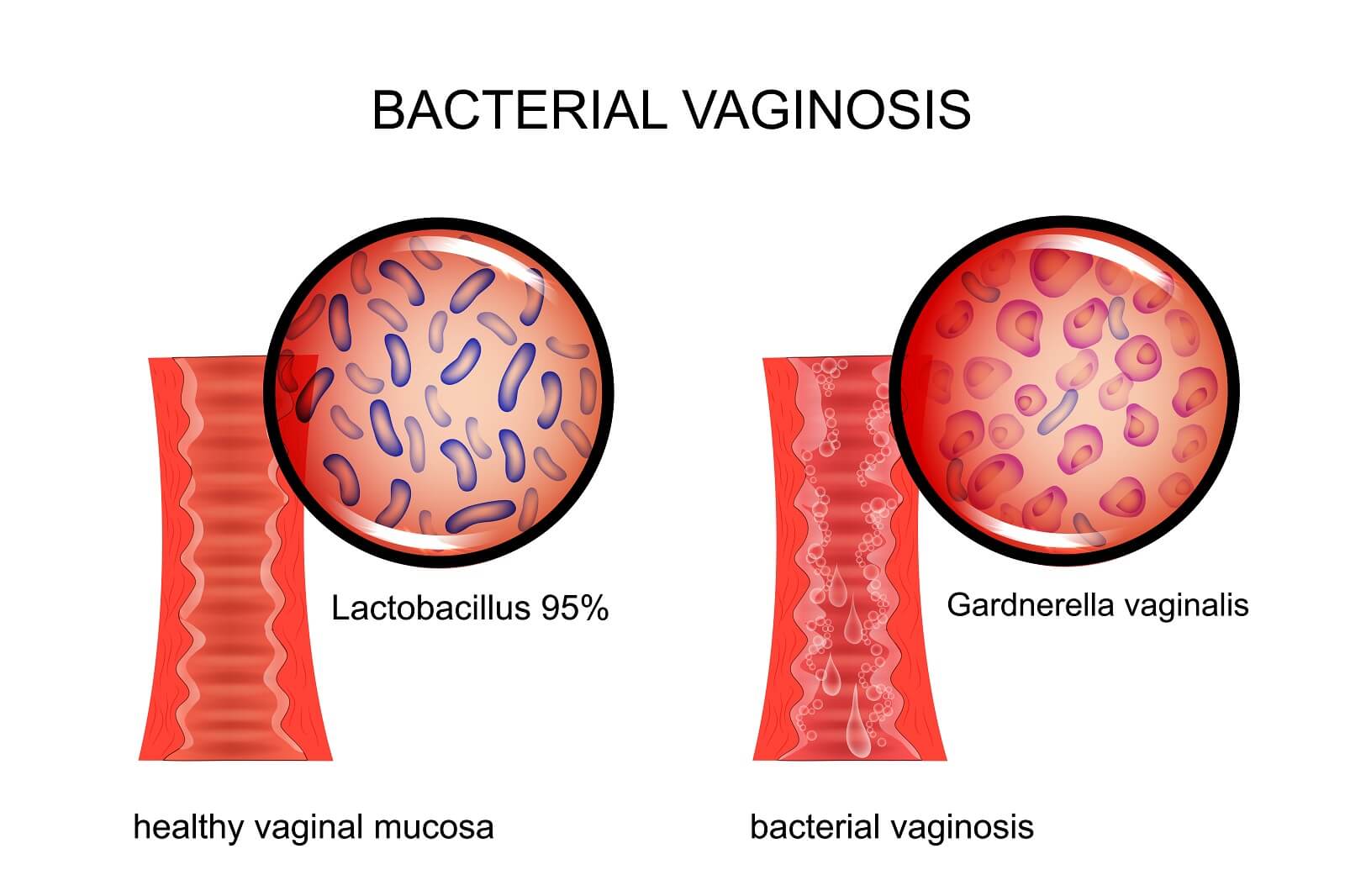
If you want to attempt a self diagnosis, the symptoms of bacterial vaginosis will be listed. Note that the fishy smell will likely be the most useful to tell if you have this; as a yeast infection will not create such an odor. Also, many women with BV don’t have any signs or symptoms at all. Also, if you have had many, or unusual, sexual partners recently; you may have the STD Trichomoniasis. Conversely, if you have had no unusual sexual activity, it is likely not an STD affecting you. The following are common bacterial vaginosis symptoms:
- A malodorous “fishy” smell emanating from the vagina; especially after sexual intercourse.
- A liquid, thin discharge from the vagina that may be greyish or whitish.
- Unusual, or strong, itching of the skin around the vagina.
- Burning sensations during urination.
Typical Yeast Infection Symptoms
If this is your first experience with what could be a yeast infection, it may be prudent to have a doctor perform some tests and come to a definite answer. If you have had a history with yeast infections; then, you probably know one when you see it. If you’d like to self diagnose your condition, here are some common yeast infection symptoms:
- A non-odorous thick, whitish vaginal discharge that is similar in consistency to cottage cheese.
- A thin, or watery, vaginal discharge.
- A rash around the vagina.
- Pain in the vaginal area, and general soreness down there.
- Swelling of the vulva, and redness of the vulva.
- Pain or a burning sensation during sexual intercourse or urination.
- General itching, or irritation of the vagina and vulva.
A Natural, 12 Hour Yeast Infection Cure

According to a research paper published in Clinical Microbiology Reviews [12.1 (1999): 80-96], Candida species are quite ubiquitous organisms. Candida are most frequently present in the mouth; and, live in 31% to 55% of healthy people. The species that causes approximately 70% to 80% of all Candida infections is C. albicans.
The Chinese Journal of Obstetrics and Gynecology [2011 Jul;46(7):496] reports there appears to be a correlation between intestinal Candida infections and vaginal yeast infections. And, this provides a clue, as to why yeast infections in general, can reoccur.
This study states, in 148 cases of vaginal candida infections, 33.1% of the women were infected in both the intestines and vaginal area. The recurrence rate of yeast infections, in women with simultaneous intestinal infection, was significantly higher than for women who did not have an intestinal infection. This study concluded that vaginal yeast infections are highly associated with simultaneous intestinal Candida infection.
As research appears to indicate, systemic Candida infections can and do happen. A more systemic Candida infection may primarily get a foothold in the intestines; and cause a wide array of problems. If your yeast infections keep happening, a systemic Candida problem may be why.
One woman who suffered from a systemic Candida infection, for about 12 years, was Linda Allen. The systemic Candida infection that attacked Linda caused a wide range of health problems in addition to yeast infections. Some of these problems, Linda describes in her own words in the following quote:
To be honest, it was hard to pinpoint exactly what was wrong: I wasn’t really sick, but I wasn’t really well either. I had listlessness, fatigue, brain fog, stomach ailments, unexplained rashes, skin infections, and so on. It seemed like every day brought a new challenge.
My energy was sapped and I felt exhausted, which affected my grades and put a big dent in my social life.
Linda Allen’s symptoms included an embarrassing vaginal discharge, severe itching, and burning sensations. Her infections were difficult to deal with, and Linda’s health problems cost her financially as well. Linda states these infections of Candida can become excruciating when they happen as frequently as a menstrual period.
Yet, Linda spent a great deal of time in research; and even questioned health professionals who were kind enough to share some time with her. Linda even tried an array of purported "cures." Although it took a while, eventually, Linda put together a natural treatment plan she hoped would solve her Candida situation.
After spending about a year refining her new approach, Linda tried her system on herself. It worked amazingly well. Linda even returned to a few medical doctors to get tested for the presence of infections. These tests revealed all indicators of infection had vanished! Linda was indeed well again, after such a long, difficult journey.
Linda has since published a book detailing how to copy her success. She also includes a 12 hour yeast infection cure that can get rid of a superficial (such as a genital yeast infection or oral thrush) yeast infection in about 12 hours.
Linda’s publisher protects those who get her book with a 60 day, 100% money back guarantee. Linda’s publisher, a subsidiary of the United States based firm Keynetics Incorporated, is a reputable digital retailer that has been around for a long time. They have great customer service, and make getting a full refund on Linda’s book quick and easy. If you’re not satisfied, you can quickly get all your money back.
If you would like to learn more about Linda’s journey to freedom from Candida, see reviews of others who tried her natural system, or find out more about her efficacious book; you can find more information at Linda Allen’s website.
Author: Mr. Nicholas Gross

Nick Gross is a natural medicine enthusiast who has been researching and writing about natural medicine since 2008. Nick is primarily a web developer but also researches and authors written and video content about natural health. Nick has a bachelor’s degree in Management Information Systems from the University of Northern Iowa.
Disclaimer
The information on this website is not a prescription for anyone. This information is for informational or educational purposes only, and is not a substitute for professional medical advice or consultations with healthcare professionals.
Affiliate Disclosure
Some of the links provided on this website are affiliate links. When a purchase is made through these links, Candida Hub earns money from commission. This helps to keep the website up and helpful to people for free. Thank you for any support!
Stay Up to Date
If you enjoyed this article, consider following / liking our Facebook page. This page is primarily utilized to alert followers of new articles that are put on Candida Hub. Candida related news is also discussed. While you are there, you can see what has been more recently added to Candida Hub.
SOURCES:
- http://dx.doi.org/10.1155/S1064744901000369 — Linhares, Iara M., et al. "Differentiation between women with vulvovaginal symptoms who are positive or negative for Candida species by culture."Infectious diseases in obstetrics and gynecology 9.4 (2001): 221-225. PDF Available Here
- https://doi.org/10.4102/hsag.v6i1.54 — Botha, D. E., and R. Van der Merwe. "Diagnosis of vaginal infection in pregnancy: research." Health SA Gesondheid 6.1 (2001): 21-27. Full Text PDF
- https://doi.org/10.1128/CMR.12.1.80 -- Fidel, Paul L., Jose A. Vazquez, and Jack D. Sobel. "Candida glabrata: review of epidemiology, pathogenesis, and clinical disease with comparison to C. albicans." Clinical Microbiology Reviews [12.1 (1999): 80-96].
- https://pubmed.ncbi.nlm.nih.gov/22041440/ -- Lin XL, Li Z, Zuo XL. "Study on the relationship between vaginal and intestinal candida in patients with vulvovaginal candidiasis." Chinese Journal of Obstetrics and Gynecology (Zhonghua fu chan ke za zhi). [2011 Jul;46(7):496].







