See all "Acidopilus" Section Topics
Does Lactobacillus acidophilus (L. acidophilus) help regulate and treat yeast infections? The answer is: it most certainly does.
Vaginal yeast infections may primarily get a foothold in the vagina when the normal bacterial life, that typically keep the yeast in check, are disrupted and reduced. Lactobacilli bacteria make up the largest segment of the bacterial life in the vagina. Species of the L. acidophilus complex are usually thought to comprise the majority of the Lactobacilli in the vagina (Vásquez, Alejandra, et al.; 2002).
These critical Lactobacilli are known to play a crucial role in protecting the urogenital system from infections. And, thus, ingesting a powerful dose of these probiotics, or inserting the probiotics directly into the vagina can help prevent yeast infections.
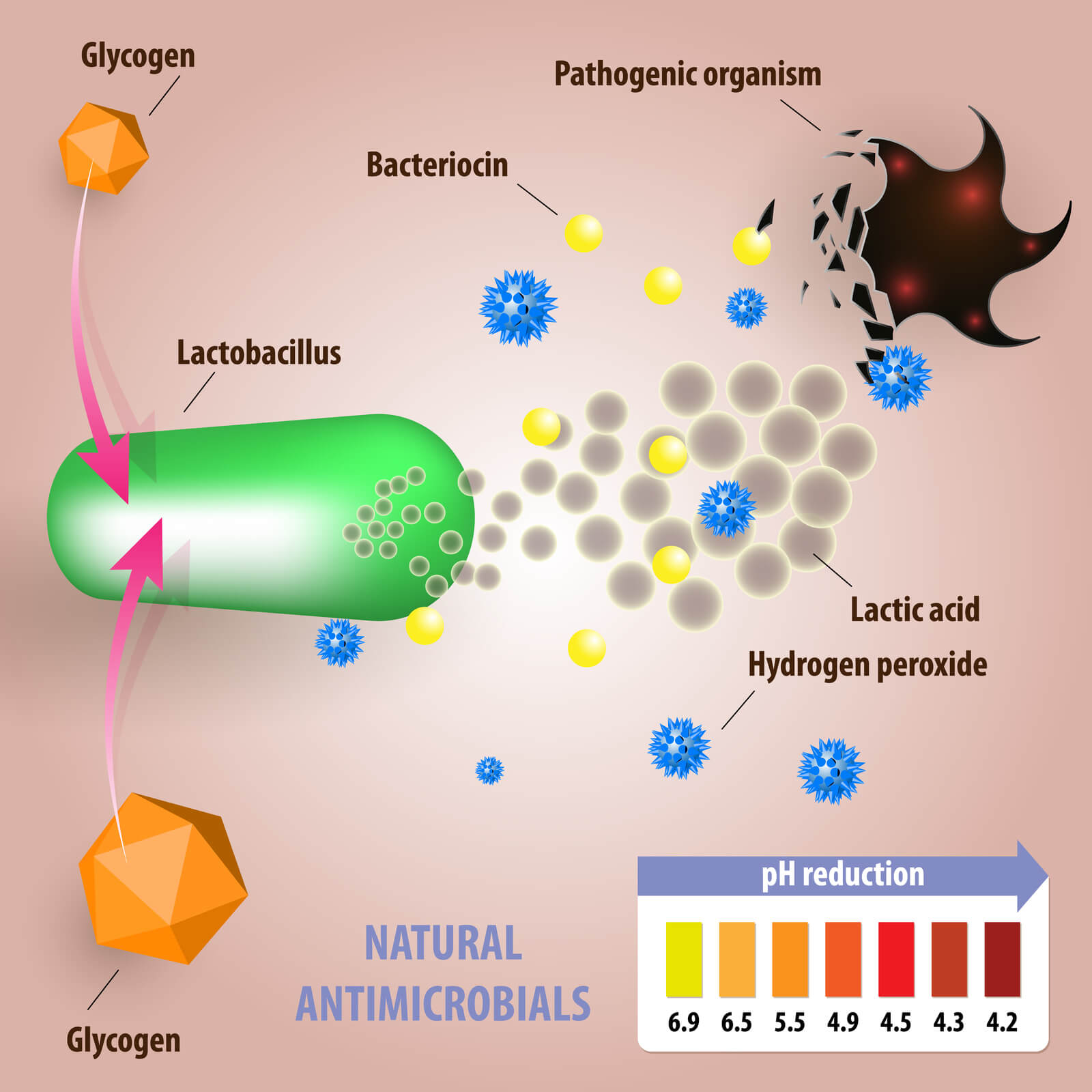
So, why does L. acidophilus work as a yeast infection treatment? The presence of this bacteria in the vagina will cause there to be less food for yeast to eat; thus, lessening the ability of the yeast to multiply. L. acidophilus can also secrete lactic acid as a by product of its metabolism; this keeps the vagina in a more acidic state. And, Candida do not like a vagina that is acidic.
Lactobacillus also attach to the walls of the vagina and take up space there—which prevents the yeast cells from latching on to the vaginal tissue and then colonizing that area. Also, Lactobacilli can create chemicals that are toxic to pathogenic bacteria; these are known as bacteriocins.
Thus, probiotics can bring the fight to yeast on several fronts; making them a great choice to supplement any natural yeast infection therapy.
To start using L. acidophilus, you can find a probiotic supplement that contains this species. It may be wise to see other species in the Lactobacillus genus included with the probiotic as well. Then, just take them orally as the package instructs you too; and, you can insert them into the vagina on a regular basis as well.
You may have to employ some other Candida killing natural items in your treatment plant to start eradicating the yeast. Then, after you kill off the yeast, these probiotic bacteria will move in and help to keep the yeast from coming back again.
A 1/2 Day & Yeast is Gone!
Linda Allen suffered from yeast infections for years. Through researching natural medicine & Candida, she found an efficacious solution!
Linda is one expert you want on your side! Let her show you how to get rid of a superficial yeast infection in just 12 hours; AND, keep it gone!
A 60-day, 100% money back guarantee is provided.
Visit Official Site!Lactobacillus Acidophilus Research

A study, published in The Indian Journal of Medical Research [129.6 (2009): 628-630], discussed the importance of Lactobacilli in the human alimentary canal and urogenital tract. The research states the probiotic organisms in the body proved resistance against potential pathogenic organisms.
Lactobacilli help to prevent pathogens from colonizing critical areas of the body by producing hydrogen peroxide, acids, and bacteriocins (a protein toxin that is harmful to other bacteria). Lactobacillus play a key role in vaginal health; and, are the predominant genus of bacteria in a healthy vagina.
When these probiotic Lactobacilli are reduced, often through antibiotics, other pathogenic anaerobic bacteria and yeast can begin to dominate the vaginal microbiota. The result can be bacterial vaginosis (BV) or yeast infections; and, BV is the most common vaginal infection.
The study states that in vitro (in glass; i.e., not in the body) experiments have revealed that Lactobacillus rhamnosus has strong efficacy in preventing Candida biofilm formation, adhesion to surfaces; and, could inhibit Candida overgrowth. A combination of Lactobacillus species can prove to be a better probiotic therapy. And, in the past, the L. acidophilus complex could not be accurately distinguished.
However, now it has been divided into the following six species: L. johnsonii, L. gallinarum, L. acidophilus, L. amylovorus, L. crispatus and L. gasseri. Thus, you may want to look for these specific species when reviewing probiotic supplements.
Another study also discussed the importance of probiotics for the control of fungal infections; this research was published in the journal Mycoses [56.3 (2013): 204-211]. The study states that the use of broad spectrum antibiotics can kill off the bacteria that live on the surface of the gastrointestinal tract and help to maintain the mucous barriers of the tract.
Fungus, such as yeast, are not affected by antibiotics; and, persist after antibiotic regimens. Since Candida is an opportunistic pathogen, the removal of the bacteria which normally kept it in check, will provide it with a significant opportunity to dominate these areas in the body.
The replenishing of these probiotics in the body, along with the aid of a healthy immune system, can be critical in the prevention of yeast infections. Orally consuming a supplement with high amounts of probiotic bacteria can rebalance the body’s microbiota. As such, probiotics like L. acidophilus, can serve as a tool in the prevention of yeast infections.
The research states that various studies have all shown probiotics can help to prevent Candida colonization and inhibit this yeast’s growth. One particular study revealed that mice with weak immune systems, when given probiotics orally and anally, were better defended against Candida.
The probiotics lowered the amount of Candida albicans in their gastrointestinal tract, reduced the rate of systemic Candida infection, and extended the survival of these mice (Wagner, R. Doug, et al.; 1997).
Also, the probiotic Saccharomyces boulardii has shown to reduce Candida albicans induced inflammation in the human intestinal wall and inhibit this yeast’s ability to attach to surfaces. Saccharomyces boulardii has also been shown to reduce Candida albicans transition to its hyphal, germ tube state.
This study also cites research that found women who were treated with Lactobacillus fermentum and Lactobacillus rhamnosus for 60 days had an increased amount of vaginal Lactobacillus bacteria.
Additional research revealed that L. acidophilus use lowered the effect of fungal growth in patients with ulcerative colitis and gastric ulcers, and generally reduced the length of time fungus colonized the gastrointestinal mucous membranes. Finally, another study showed that taking probiotics can help prevent intestinal colonization by Candida.
One excellent study took a look at exactly how well eating L. acidophilus rich yogurt would impact women who suffered from recurrent vaginal yeast infections. This research was published in the Annals of Internal Medicine [116.5 (1992): 353-357]. Women who were on a strong antibiotic therapy, were receiving immunosuppressive therapy, who had multiple pathogens in their vagina, or who had been eating 16 ounces of yogurt weekly were not allowed to participate in the study.
The yogurt used was verified to contain live L. acidophilus cultures; and, the women eating the yogurt, ate 8 ounces of it daily. In one arm of the study, the women ate yogurt for extended periods of time, and then ceased eating the yogurt. In the other arm, women started out not eating yogurt and then started eating yogurt after a certain time.
The patients in the study were seen at monthly intervals for a minimum of a year’s time. At each monthly checkup, the participants were examined and microbiological tests were carried out.
The researchers found, that when women consumed yogurt with live L. acidophilus, their rate of developing yeast infections went down three-fold. The rate of Candida colonization in the women who ate the acidophilus yogurt dramatically dropped—being much less than those who did not eat the yogurt.
The study also found a very strong correlation regarding the presence of L. acidophilus in the rectum and in the vagina. When L. acidophilus was present in the recutum, there was a strong increase in the probability it would be found in the vagina.
Another study shows L. acidophilus is capable of inhibiting Candida growth; and, the resulting chemical material from this bacteria’s fermentation process can kill Candida. The study was published in International Journal of Antimicrobial Agents [Volume 26 , S80]. The study found a strain of L. acidophilus was able to inhibit a wide range of bacteria, Candida albicans, and other fungi.
This strain of L. acidophilus produced lactic acid. And, the fluid that formed on top of the medium on which this bacteria was grown on for 48 hours was able to inhibit Candida albicans. This fluid also was able to kill Candida albicans cells. The study concluded that L. acidophilus has potential as being used as an antimicrobial.
Another study looked at the ability of probiotic, vaginal Lactobacillus bacteria to counter Candida. The research was published in Infectious Diseases in Obstetrics and Gynecology [13.2 (2005): 69-75]. The study relates that Lactobacilli are a key part of the vaginal microbiota; and, these bacteria are the dominant microorganism in the vaginas of healthy women who have not entered menopause.
The reduction of Lactobacilli in the vagina is associated with vaginal maladies like urinary tract infections and bacterial vaginosis. Essential operations of Lactobacilli, that grant it its protective powers, include the synthesis of hydrogen peroxide, the ability of some strains to readily attach to the walls of the vagina, the production of chemicals toxic to other types of bacteria, and the production of acid products—such as lactic acid.

The study used plates with a growth medium on them and placed Candida albicans and strains of Lactobacillus in the plates. The research showed that all of the strains of Lactobacillus inhibited the growth of Candida albicans to some extent.
L. acidophilus always totally inhibited the growth of Candida albicans in the direct area where it was placed on the dish. And, two of the five L. acidophilus strains prevented growth of Candida albicans beyond the direct area the bacteria grew on.
The study concludes that the proper application of the correct strains of Lactobacillus in the vagina may be of value in preventing various genitourinary diseases. The following quotation was taken from the study.
Certain strains of Lactobacillus genus, isolated from the vagina and representing major species colonizing vaginal mucosa of healthy women, express distinct adherence and antagonistic properties in vitro which may indirectly indicate their protective role in stabilizing the vaginal microflora and controlling other members of the vaginal flora, including Candida albicans. It seems that inhibition of C. albicans by different Lactobacillus strains is dependent on various mechanisms.
http://dx.doi.org/10.1080/10647440400028136
Eliminate Bacterial Vaginosis & Vaginal Odor
Jennifer O’Brien is one prominent expert on BV that knows how to get rid of vaginal odor. BV is a common infection that you don’t have to put up with.
Jennifer will show you how to naturally eliminate vaginal odor in just 3 days.
A 60-day, 100% money back guarantee is provided.
Visit Official Site!Survival of L. acidophilus in Stomach Conditions
One study looked at the viability of L. acidophilus bacteria in an artificial gastric juice. The research was published in Food Hydrocolloids [20.8 (2006): 1164-1169]. The study relates that living Lactic acid bacteria (those that produce lactic acid) are consumed via fermented yogurt, cheese, milk, and other foods.
Many kinds of these bacteria have beneficial effects on people’s health, and are classified as probiotics. The study states Lactobacillus tends to reside in the lower intestine, and Bifidobacterum resides in the colon. The research makes clear these bacteria are beneficial to the immune system; and, they also help to regulate the function of the intestine.
The focus of this study was on the survival of L. acidophilus in a simulated gastric fluid. The control arm of the study, used unprotected L. acidophilus. The experimental arm of the study, used a water-in-oil-in-water (W/O/W) emulsion to protect the bacteria.
An emulsion is a suspension—such as fat in milk—consisting of a liquid dispersed, with or without an emulsifier, in a liquid usually in droplets; but, this mixture cannot be mixed. A mixture that can be mixed together would be salt and water. A simulated gastric juice mixture, to compare to conditions within the stomach, was also created. The bacteria were then placed in this mixture to determine how well they would survive.
The research found, that L. acidophilus by itself, died quite quickly—for the most part—in the simulated gastric juice. When unprotected L. acidophilus was placed into gastric juice, only 1.3% of the original bacteria were alive after about 40 minutes of time transpired.
Thus, 98.7% of the L. acidophilus were killed by the simulated gastric juice. On the other hand, those bacteria protected by the W/O/W emulsion, had a much, much better survival rate. The W/O/W emulsion protected L. acidophilus had a 49% survival rate after being in the simulated gastric juice for 2 hours of time.
Although these figures are staggering, one must remember that there are a lot of bacteria in food items with living cultures. And, since about 1.3% (or more) of these probiotic bacteria survive the digestion process; they do begin to colonize the digestive system and repopulate.
So, regularly eating foods rich in probiotic bacteria, throughout the day, will begin to enrich your gastrointestinal tract with these bacteria. And, if you eat foods that these bacteria like to eat (such as real sweet whey), they can begin to grow and form healthy, viable colonies in your digestive system.
The result, is your intestines are well shielded from pathogenic bacteria and yeast; due to the forceful presence of helpful bacteria; such as Lactobacilli and Bifidobacterum.
Another research study, also examined how well L. acidophilus would survive in simulated stomach conditions; and, then attach to the intestinal walls. The study was published in the Journal of Food Science [53.5 (1988): 1514-1516]. This study suggested that when you are trying to select a species of Lactobacilli for therapeutic effect, there are some factors that should be considered.
One factor, of great importance, is the ability of a bacteria to attach to the gastrointestinal tract; and, subsequently colonize that area. Consequently, it is important to see if, after a bacteria passes through the digestive process of the stomach, it can subsequently attach to and colonize the intestines.
The study states L. acidophilus is able to survive in gastric juice; and, survival in gastric juice had been found to be enhanced by the addition of skim milk (and, drinking something like skim milk would probably assist in the survival of these bacteria). The study sought to see how well L. acidophilus would survive at varying pH levels of 2, 3, and 4.
The research also analyzed the effect a low pH had on L. acidophilus’ ability to attach to human intestinal tissue cells in vitro (in a test environment, outside of the body).
The research found a solid correlation between the acidity of the fluid the L. acidophilus were incubated with and their survival rate. At a pH of just 2 (quite acidic), living bacteria cells rapidly decreased; none were alive after 45 minutes of this incubation. Conversely, at a pH of 4, the number of living bacteria were not significantly reduced after 2 hours of incubation.
Concerning the ability of the bacteria to attach to intestinal cells, after being subjected to low pH fluid, the research found the bacteria were able to adhere. When L. acidophilus was subjected to a low pH, and then exposed to human intestinal cells, the ability to attach to these intestinal cells did not appear to be inhibited.
L.acidophilus that was not subjected to a low pH adhered to the intestinal cells similarly to those bacteria subjected to pH levels of 2, 3, and 4 for up to 5 hours. Although, it should be noted, after 5 hours of L. acidophilus being exposed to a pH of 2, no living cells were present. These dead cells did retain their ability to attach to the human intestinal cells. Therefore; although the bacteria may have been killed, via a low pH, the dead cells were still able to attach.
Clair Goodall: Author & Nature Lover
Clair Goodall is a bee-obsessed natural medicine convert from Minnesota. She is one expert you might want to know more about!
Clair will help you protect you and your family from toxic products and chemicals and help you discover solutions from nature.
Also, Clair’s book is backed by a 60-day, 100% money back guarantee
Visit Official Site!Foods with Acidophilus

Yogurt is a typical food that comes to mind when you are considering how to introduce good bacteria into your digestive system. However, as you may know, a yogurt that doesn’t contain live probiotic cultures will not add beneficial bacteria to the digestive system.
Regular yogurt is made via fermentation with two bacteria: Lactobacillus bulgaricus and Streptococcus thermophilus. These two bacteria do not have the ability to survive through the intestinal tract. Additionally, L. bulgaricus and S. thermophilus are not amongst the normal bacterial flora of the intestines, and these bacteria are not resistant to bile acid (Gilliland, 1979).
Although these bacteria do not live in the human gut, the metabolites they produce in the fermentation of yogurt have positive effects; the metabolites aiding the digestion of lactose and inhibiting certain pathogens.
Therefore, for a yogurt to actually be a viable option as a probiotic supplement, the bacteria within it must fulfill some criteria. One study listed these criteria; it was published in the International Dairy Journal [11.1-2 (2001): 1-17]. According to the research, the criteria a bacteria must fulfill, to be considered probiotic include:
- The bacteria must be a normal inhabitant of the human intestinal system.
- Be able to colonize the digestive system at some location.
- The bacteria must be capable of surviving through the upper digestive system in significant numbers.
- The bacteria must produce a positive effect by being in the digestive system.
According to this same International Dairy Journal [11.1-2 (2001): 1-17] study; L. acidophilus and Bifidobacterium, are widely suggested by scientific studies, to have therapeutic effects. This study relates that the purported benefits from consuming probiotic products was once a highly debated issue.
Now, however, it is well known and recognised that probiotics have many beneficial effects. The research makes clear that consuming probiotic bacteria assists in maintaining good health, can mitigate intestinal disease, and can rejuvenate the body’s vigor. And, of course, many probiotic yogurts contain L. acidophilus and Bifidobacterium.
As regular yogurt bacteria is not probiotic, and cannot colonize the intestines via eating yogurt, regular yogurt is not of much benefit. You must look for yogurt that contains live cultures of probiotic bacteria.
L. acidophilus should be at the top of your list; as this bacteria is perhaps the most famous of all probiotics. And, it should be hard to find a probiotic yogurt that does not contain L. acidophilus; the species is just too beneficial and therefore quite ubiquitous to probiotic yogurt. For more information regarding yogurt and Candida, see this article: Using Probiotic Yogurt for Yeast Infections.
The same rules apply to other fermented foods; if they do not contain actual living probiotic strains of bacteria; they are of little value. Using probiotic pills, you can always add in these pill’s contents to food items, and ferment them yourself. Due to availability, you may be limited to only probiotic yogurt at your local grocery store.
Therefore, keep in mind that you can make your own fermented foods, such as kefir, at your home. Just make sure you add in good strains of bacteria that meet the criteria for being probiotic!
As you may know, foods that contain live bacteria naturally are often pasteurized. Pasteurization is the process of heating a food to kill the bacteria in it. Thus, most of the milk and yogurt you find at the grocery store will have had its bacteria wiped out a long time ago. Therefore it is vital that a product’s label state there are live cultures in the food item.
If you have some time, you can always make your own homemade yogurt that contains L. acidophilus. Just add some probiotic pills to your batch of milk before you start turning it into yogurt. After several hours pass in a yogurt maker, these bacteria will begin to rapidly multiply. Your yogurt will then contain actual live bacteria; and, you can start eating it daily and inserting it into the vagina to help allay a yeast infection.
Sweet whey also will help to feed the L. acidophilus bacteria. If you have taken a probiotic, you may want to start eating some sweet whey to deliver the bacteria in your digestive system plenty of food. For more information about this topic, you can check out: sweet whey and L. acidophilus.
Linda Allen’s 12 Hour Yeast Infection Treatment

A significant portion of women will end up suffering from recurrent vaginal yeast infections. You may even be a victim of this tragic condition yourself. One woman, Linda Allen, ended up having recurrent yeast infections early in her life. And, for about a decade thereafter, Candida would rob her of her health and well being.
Linda’s yeast related health problems started in her late teen years; about the same time she developed a sinus infections. It was around this time that Linda came down with a vaginal yeast infection. Linda wasted little time before she consulted a doctor for help. The physician quickly wrote out a prescription for her. Linda found that using this antifungal drug, her yeast infection cleared up rapidly; and, her problem appeared to be over.
But, after time passed, Linda found she had developed another yeast infection. Again, Linda went back to her doctor and got another prescription. The yeast infection again went away. Yet, it did not stay gone long; after a short while, Linda found herself infected again by Candida.
The cycle of yeast infection recurrence would last about a decade in Linda’s life. All the while Linda dealt with outward yeast infections, her general health continued to worsen. She spent a small fortune on prescription drugs and medical bills.
Doctors would prescribe her stronger and stronger antibiotics to deal with the myriad of problems she was having. And, she was even put on allergy medications to help relieve her symptoms. Yet, these drugs only improved her condition temporarily; they never offered her a complete, permanent solution.
Those who knew Linda began to wonder if she was just sicker than she was letting on; or, perhaps she was a little bit of a hypochondriac. All of Linda’s medical bills began to add up; she could have bought her first house with the money she put into fixing her health!
Linda’s life did change for the better one fateful day, when she decided to visit a naturopath about her health. The naturopath knew exactly what was going on with Linda’s body and told her she was suffering from systemic yeast overgrowth. The naturopath was not able to totally end Linda’s yeast problems; but, it was a revelation that gave her a starting point to go from.
Linda began to become very interested in holistic, natural medicine. She bought a host of medical books and spent an extended amount of time studying them. When Linda found a doctor or medical expert willing to lend her some time, she consulted them for advice. Linda tried a wide array of alternative methods for curing Candida; and, although none worked totally, they occasionally provide her with key insights.
Eventually, Linda began to correlate her experience with these natural treatments and applied her knowledge of Candida to arrive at a powerful treatment plan. Linda spent a year polishing and perfecting her new approach. The time finally came when Linda applied her new approach to herself. Linda found that she began to rapidly improve after starting this new therapy.
Her vaginal yeast infections went away; and, as time went on, her health improvements did not dissipate. Eventually Linda felt like her old, healthy self again! Linda gave others her new method and they too found that all their symptoms would melt away quickly using her therapy. Linda had finally arrived at a permanent, safe, and natural cure for her Candida problem.
Linda has since published a book detailing her entire Candida treatment program. Linda guarantees that oral and genital yeast infections will be totally cured in just 12 hours time using the method outlined in her book.
And, after a few weeks have passed; even stubborn, systemic Candida overgrowth will be eradicated from the body! Since Linda’s book was published in 2004, over 100,000 individuals from around the world have seen amazing results using Linda’s treatment.
Linda Allen’s book is published by a large, reputable online retailer—which is owned by the U.S. based firm Keynetics Incorporated. Linda’s publisher has been doing business since nearly the advent of the internet; and, you can be assured of a safe, easy purchase.
And, Linda guarantees her her 12 hour cure time for oral and genital yeast infections; if they don’t go away in half a day, you can get all your money back by making a quick request to Linda’s publisher. Linda’s book is available as a digital ebook you can download instantly if you decide to give it a try! There is no need to return anything if you request a refund.
To learn a bit more about Linda’s personal story and journey to better health, to see testimonials from many happy people who tried Linda’s book, or to see some of the free bonus books she offers with her’s, you can find out more information any time at Linda Allen’s website.
Author: Mr. Nicholas Gross

Nick Gross is a natural medicine enthusiast who has been researching and writing about natural medicine since 2008. Nick is primarily a web developer but also researches and authors written and video content about natural health. Nick has a bachelor’s degree in Management Information Systems from the University of Northern Iowa.
Disclaimer
The information on this website is not a prescription for anyone. This information is for informational or educational purposes only, and is not a substitute for professional medical advice or consultations with healthcare professionals.
Affiliate Disclosure
Some of the links provided on this website are affiliate links. When a purchase is made through these links, Candida Hub earns money from commission. This helps to keep the website up and helpful to people for free. Thank you for any support!
Stay Up to Date
If you enjoyed this article, consider following / liking our Facebook page. This page is primarily utilized to alert followers of new articles that are put on Candida Hub. Candida related news is also discussed. While you are there, you can see what has been more recently added to Candida Hub.
SOURCES:
- http://dx.doi.org/10.1128%2FJCM.40.8.2746-2749.2002 — Vásquez, Alejandra, et al. "Vaginal Lactobacillus flora of healthy Swedish women." Journal of clinical microbiology 40.8 (2002): 2746-2749. PubMed Full Text
- http://www.ncbi.nlm.nih.gov/pubmed/19692740 — Sethi, Sunil, Gagandeep Singh, and Meera Sharma. "Lactobacilli as probiotics against genital infections." The Indian journal of medical research 129.6 (2009): 628-630. PDF Available Here
- http://dx.doi.org/10.1111/myc.12021 — Kumar, Suresh, and Sunit Singhi. "Role of probiotics in prevention of Candida infection in critically ill children." Mycoses 56.3 (2013): 204-211. PubMed
- http://www.ncbi.nlm.nih.gov/pmc/articles/PMC175599/ — Wagner, R. Doug, et al. "Biotherapeutic effects of probiotic bacteria on candidiasis in immunodeficient mice." Infection and immunity 65.10 (1997): 4165-4172. PDF Available Here
- http://dx.doi.org/10.7326/0003-4819-116-5-353 — Hilton, Eileen, et al. "Ingestion of yogurt containing L. acidophilus as prophylaxis for candidal vaginitis." Annals of Internal Medicine 116.5 (1992): 353-357. PubMed
- http://dx.doi.org/10.1016/S0924-8579(05)80225-0 — “A7.6 Novel biotherapeutics from L. acidophilus USTCMS 1073 exhibiting potent inhibitory activity against bacteria, filamentous fungi and Candida albicans.” International Journal of Antimicrobial Agents , Volume 26 , S80. PDF Available Here
- http://dx.doi.org/10.1080/10647440400028136 — Strus, Magdalena, et al. "The in vitro activity of vaginal Lactobacillus with probiotic properties against Candida." Infectious diseases in obstetrics and gynecology 13.2 (2005): 69-75. PubMed PDF
- https://doi.org/10.1016/j.foodhyd.2006.01.001 — Shima, Motohiro, et al. "Protection of Lactobacillus acidophilus from the low pH of a model gastric juice by incorporation in a W/O/W emulsion." Food Hydrocolloids [20.8 (2006): 1164-1169].
- https://doi.org/10.1111/j.1365-2621.1988.tb09312.x — Hood, S. K., and E. A. Zoitola. "Effect of low pH on the ability of Lactobacillus acidophilus to survive and adhere to human intestinal cells." Journal of Food Science [53.5 (1988): 1514-1516].
- https://doi.org/10.4315/0362-028x-42.2.164 — Gilliland, S. E. (1979). Beneficial inter-relationships between certain microorganisms and humans: Candidate microorganisms for use as dietary adjuncts. Journal of Food Protection [42, 164-167].
- https://doi.org/10.1016/S0958-6946(01)00036-X — Lourens-Hattingh, Analie, and Bennie C. Viljoen. "Yogurt as probiotic carrier food." International Dairy Journal [11.1-2 (2001): 1-17].








